 |
A simple air filter could cut indoor pollution in half and even lower your blood pressure if it’s already on the high side.
In a new study, researchers enrolled adults living within 200 meters of a highway. Each person had one month with real HEPA filters in their bedroom and living room and one month with sham filters (same look and sound, no filter).
Indoor particulate matter levels dropped by ~50% with HEPA filters and particle counts fell from ~6,300 to ~4,700 particles/cm³. The biggest improvements came midday and in the evening—times when indoor cooking can spike particles.
Overall, there was no significant group-wide effect on blood pressure (only a small 0.5 mmHg reduction compared to the sham condition), but among people with systolic BP ≥120 mmHg, HEPA use lowered systolic BP by ~3 mmHg.
In today's email, we'll explore this study, discuss the other impacts of air pollution on cardiovascular health and beyond, and talk about what you can do to mitigate your risk.
You just missed this in your inbox
Every week, Dr. Rhonda Patrick and the FoundMyFitness team distill the latest research into clear, actionable insights on health, longevity, and performance, delivered free to your inbox.
Cleaner Air Means Lower Blood Pressure
The randomized crossover study, published in the Journal of the American College of Cardiology, pragmatically investigated whether in-home high-efficiency particulate air (HEPA) filtration could improve blood pressure and indoor air quality for residents living near high-traffic highways. The trial enrolled 154 adults living in Massachusetts, all residing within 200 meters of a major roadway—an environment associated with higher exposure to traffic-related air pollution.
Each participant underwent two one-month interventions in their home separated by a one-month washout period.
-
Active HEPA filtration, with devices placed in the bedroom and living room.
-
Sham filtration, in which identical-looking and -sounding devices were installed but without an actual filter.
The participants were blinded to which condition they were receiving (important to rule out any potential placebo effects). Blood pressure was measured in the morning, in the participants’ homes, both before and after each intervention phase. In a subset of homes, researchers also measured fine particulate matter (PM₂.₅) and particle number counts to evaluate the filters’ effectiveness throughout the day.
HEPA filtration significantly reduced indoor air pollution compared with both outdoor air and sham filtration. Average PM₂.₅ concentrations were 3.0 μg/m³ in outdoor air, 5.2 μg/m³ in unfiltered indoor air, and 2.5 μg/m³ in HEPA-filtered indoor air. This represented roughly a 50% reduction in indoor PM₂.₅ compared with the sham condition. Particle number values also declined from 10,052 particles/cm³ outdoors to 6,295 indoors during the sham period and 4,706 with HEPA filtration. The largest reductions occurred around midday and in the early evening (6–9 PM), times typically associated with indoor cooking and higher particulate generation.
|
|
|
The effects of HEPA filtration and sham filtration on blood pressure in participants with blood pressure of 120 mmHg and above and below 120 mmHg. |
| |
When looking at the entire cohort, HEPA filtration had no significant effect on blood pressure, which was non-significantly reduced by 0.5 mmHg compared to the sham condition. However, an analysis using different blood pressure cutoffs revealed an interesting pattern.
Among the participants with baseline systolic blood pressure ≥120 mmHg, HEPA filtration reduced systolic BP by approximately 3 mmHg compared with the sham condition, while no effect was observed on diastolic BP. The benefit plateaued at a starting systolic BP of 120 mmHg and remained consistent up to 130 mmHg.
In contrast, participants with baseline systolic BP <120 mmHg experienced no measurable change. Those who spent more than 22 hours per day indoors showed a non-significant trend toward greater benefit (–1.7 mmHg vs. sham), though the authors note that this exploratory outcome should be interpreted with caution. It's an interesting finding nonetheless.
These moderate-term effects mirror prior research showing that traffic-related air pollution can acutely raise blood pressure. Even one hour of exposure to high pollution can elevate systolic BP by ~3 mmHg, while lower levels of pollution still cause increases of 0.5–1.5 mmHg.
The findings suggest that in-home HEPA filtration can reduce indoor air pollution for individuals living near high-traffic areas, with modest but potentially clinically relevant reductions in systolic blood pressure among people with elevated blood pressure, especially those spending a lot of time inside.
Does this mean that an air filter isn't helpful for those without high blood pressure? Certainly not—but it does suggest that people with a less favorable cardiovascular risk profile may stand to benefit more from using one.
The same thing could be said for cognitive decline. While air pollution in general is associated with a greater risk of dementia and Alzheimer's, people with one or more copies of the APOE4 allele experience greater cognitive decline when exposed to pollution than non-carriers. This increased susceptibility means that limiting air pollution exposure is especially prudent for at-risk individuals—using an air filter should be a non-negotiable.
As we'll see, there are many other reasons why it's a good idea to reduce your exposure to indoor (and outdoor) air pollution.
|
|
|
|
The effects of HEPA filtration on particulate matter at different hours of the day. |
| |
Our most recent Aliquot episode (#132) goes in depth on strategies to mitigate the harms of air pollution for you and your family, including supplements, air filtration, and green spaces.
-
03:12 - Air pollution's overlooked role in Alzheimer's and autoimmunity
-
07:29 - The environmental exposures most linked to chronic disease
-
09:30 - Clearing air pollutants with sulforaphane and sauna
-
11:15 - How city living may amplify dementia risk
-
16:01 - Could omega-3 and air filtration protect the brain from pollution
-
16:55 - What really matters when choosing an air filter
-
26:07 - Why green spaces matter in polluted environments
|
|
Air Pollution as a Cardiovascular Risk Factor and Beyond
Air pollution is recognized as a modifiable risk factor for cardiovascular disease. Both short-term spikes and long-term exposure to fine particulate matter (i.e., PM₂.₅) increase cardiovascular risk, even at levels many would consider “clean.” Large U.S. cohort studies and even meta-analyses consistently link long-term PM₂.₅ exposure to higher rates of cardiovascular disease events and mortality, estimating as much as a 10–15% increase in cardiovascular mortality for every 10 μg/m³ rise in annual PM₂.₅ exposure. Importantly, these risks persist at concentrations below historical U.S. air quality standards. There's probably no real "safe" level of exposure.
The biological mechanisms are well established. PM₂.₅ drives oxidative stress, systemic inflammation, and endothelial dysfunction and disrupts autonomic control, increases blood coagulability, and accelerates atherosclerosis, creating multiple pathways to cardiovascular harm that likely explain why cardiovascular disease risk is higher in people exposed to more air pollution (and even why short-term spikes can elevate heart attack and stroke risk).
In addition to cardiovascular disease, chronic air pollution has also been linked to a greater risk of dementia, type 2 diabetes, lung cancer (including in never smokers), pregnancy outcomes (e.g., preterm birth and low birth weight), and chronic kidney disease.
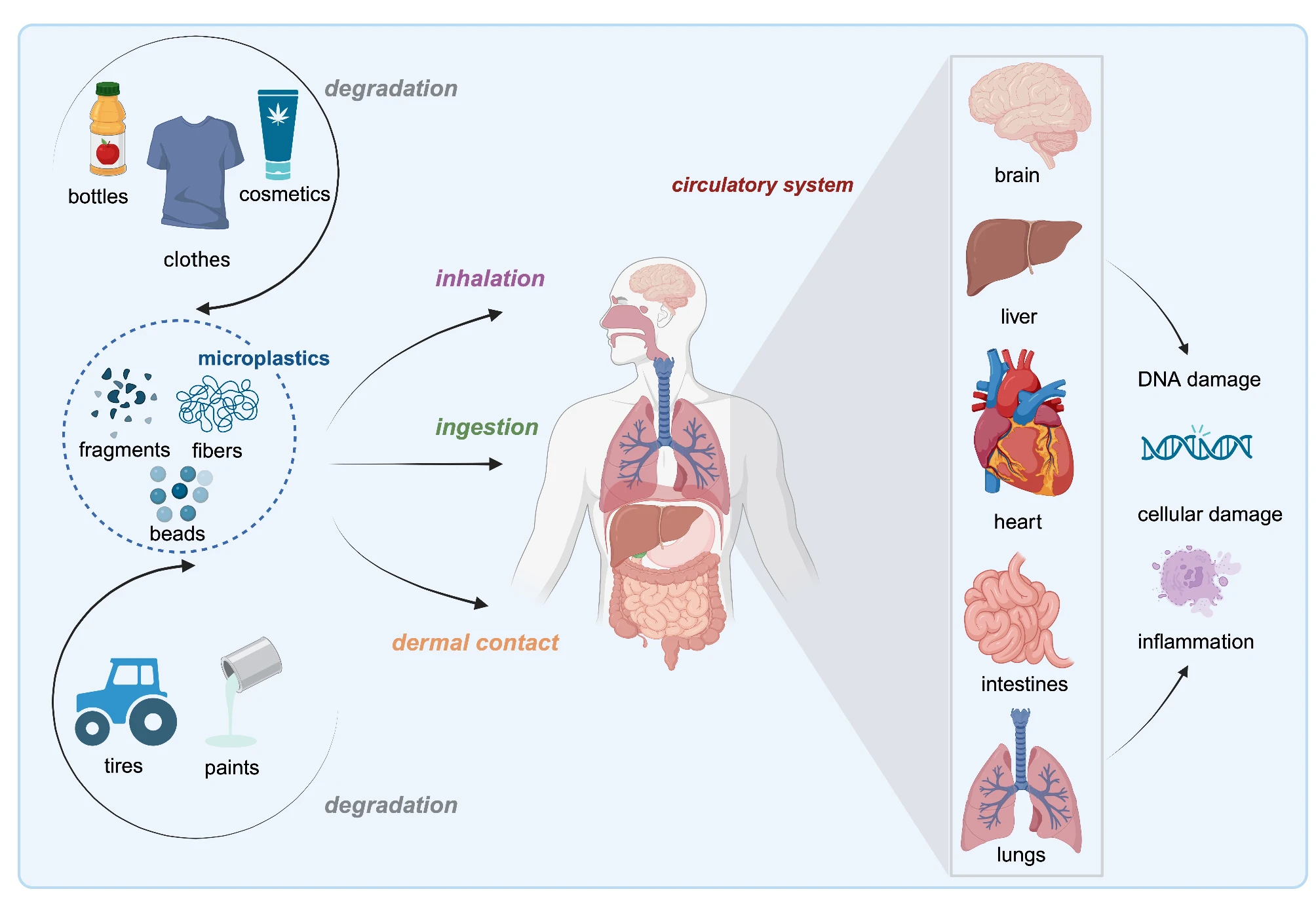
Traffic-related air pollution is a major concern, but it’s not the only one. Indoor and outdoor air can also carry harmful particles such as microplastics. Recent estimates suggest inhalable microplastic particles (1–10 μm) may be 100 times higher than previously thought, potentially leading to the inhalation of up to 68,000 particles per person per day. Inhaled particles—especially microplastics—are particularly worrisome because they can bypass the digestive tract and reach the brain directly via direct transport from the nasal passages along the olfactory nerve (bypassing the blood–brain barrier) and, after they deposit in the lungs, passage into the bloodstream where they can cross into brain tissue. Startling data from Mexico City (where air pollution levels are far above WHO and EPA standards) reveals signs of Alzheimer's disease, including neuroinflammation, neurodegeneration, cognitive impairment, and amyloid deposition in adults under 30 and even children as young as 11 months old.
Minimizing spikes in ultrafine particle exposure and maintaining clean indoor air are reliable strategies for safeguarding cardiovascular, metabolic, and neurological health at every stage of life.
|
|
| |
Final Thoughts
We don't often think of the air we breathe as a health lever that we can control—but it is, at least to some extent.
Even if you don't live near a highway or area where exposure to traffic-related air pollution is a concern, investing in a high-quality HEPA filter seems wise. Air pollution from traffic sources is just one of many types of exposures we're subjected to on a daily basis—all of which can potentially affect our long-term health.
Air filters may also have other benefits such as improving sleep by reducing CO2 levels—a hidden source of sleep disruption (Dr. Andy Galpin explains why on episode #101 of the podcast). An air filter can help bring CO2 levels down (ideally below 900 ppm) before sleep and improve the quality of the air at the same time. People with a sensitivity to airborne allergens might get a notable benefit from a filter at night too.
HEPA filters aren't cheap, but they represent a worthwhile investment for those looking to optimize the air quality in their home. However, they aren't the only option; things like sulforaphane and omega-3 supplementation and access to green spaces (strategies I explore in our most recent Aliquot episode) may also be effective.
Warm regards
— Rhonda and the FoundMyFitness team
|
|
|
|
|
|