 |
You've probably heard of metformin. It's a popular and effective diabetes medication that's also been talked about as a "longevity drug" in some circles.
But its benefits may come with an unintended side effect.
Combining metformin with exercise interferes with the usual improvements in aerobic fitness, metabolism, muscle strength and hypertrophy, and—as shown in a recent study—blood vessel function.
Adults performing low- or high-intensity aerobic exercise for 16 weeks while taking the standard clinical dose of metformin showed no improvement in their VO2 max, while those on placebo improved by about 6% on average.
Metformin also blunted increases in macrovascular and microvascular insulin sensitivity seen with both exercise intensities, attenuated improvements in fasting blood glucose, and prevented gains in whole-body insulin sensitivity, even after high-intensity exercise.
This is not isolated; other trials show metformin interferes with multiple exercise adaptations, likely via inhibition of mitochondrial complex I, which disrupts cellular energy sensing.
Metformin remains an excellent, safe first-line therapy for type 2 diabetes.
But caution is warranted when using it as a general “longevity drug," especially if it interferes with the single most powerful longevity intervention we have—exercise.
In today's newsletter, I'll break down this study, discuss why metformin may be having this effect, and unpack why we should be cautious about any bold claims about lifespan-extending benefits of metformin.
|
 |
You just missed this in your inbox
Every week, Dr. Rhonda Patrick and the FoundMyFitness team distill the latest research into clear, actionable insights on health, longevity, and performance, delivered free to your inbox.
Metformin Interferes with Exercise
The study, published in The Journal of Clinical Endocrinology and Metabolism, included 72 adults who were at risk for metabolic syndrome, which was defined by having at least 3 metabolic syndrome risk factors (e.g., elevated blood lipids, waist circumference, blood pressure, HbA1c or a family history of cardiometabolic disease).
The participants were randomly assigned to one of four groups for 16 weeks:
Low-intensity exercise + placebo Low-intensity exercise + 2,000 mg/day of metformin High-intensity exercise + placebo High-intensity exercise + 2,000 mg/day of metformin
Exercise intensity was set at 55% of each participant's VO2 max for the low-intensity group and 85% for the high-intensity group. The participants performed 3 supervised and 2 unsupervised training sessions per week.
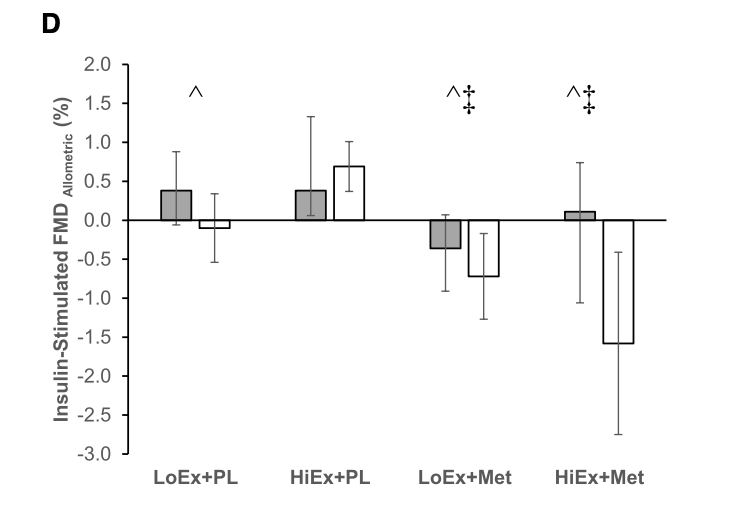
Vascular insulin sensitivity (the main outcome) was measured using a technique known as flow‑mediated dilation or FMD, which is just a way of saying how much a large artery can widen when it’s asked to handle more blood. In this study, they looked at that widening while insulin was present, so it reflects how insulin‑sensitive the large vessels are. They also measured microvascular blood flow—how many of the smallest blood vessels in the muscle are open and how much blood is getting through them when insulin is around.
The results consistently demonstrate that metformin interferes with several metabolic and vascular adaptations typically induced by exercise training.
For one, metformin blocked any improvements in aerobic fitness: both the low- and high-intensity exercise groups taking the placebo improved their VO2 max after 16 weeks (about a 6% change from pre to post), but neither of the groups taking metformin showed a significant change in VO2 max. The drug prevented the expected improvements in cardiorespiratory fitness.
The combination of metformin and exercise was also less effective for key metabolic health markers than exercise alone—improvements in fasting blood glucose were attenuated and whole-body insulin sensitivity showed no change, even after high-intensity exercise (in contrast, high-intensity exercise + placebo improved insulin sensitivity the most of any intervention).
But the central finding was that metformin diminished improvements in vascular insulin sensitivity that normally occur with exercise.
Exercise + placebo groups showed marked improvements in macrovascular function. Metformin blunted this response in both low- and high-intensity exercise groups. Likewise, the improvements in microvascular blood flow after 16 weeks of exercise training were significantly less when exercise was combined with metformin.
This was true even for the participants engaging in high-intensity exercise, which was the most effective for enhancing macro- and microvascular function.
One area where metformin didn't interfere was body composition—body weight dropped in all groups by around 2–6 lb, body fat percentage decreased by about 1% on average, and waist circumference (a marker of visceral fat) decreased by about 2–3 cm.
It's important to note that the participants did not get worse or fail to improve vascular insulin sensitivity with exercise + metformin, they just got less benefit than they would have from exercise alone. But that's still important—improvements in vascular function are one of the hallmark adaptations to exercise and explain much of why it's so beneficial for cardiovascular and metabolic health. It's not something we want to be interfering with.
|
|
Why Metformin Dampens Exercise's Effects
One of the key questions is how metformin attenuates training adaptations.
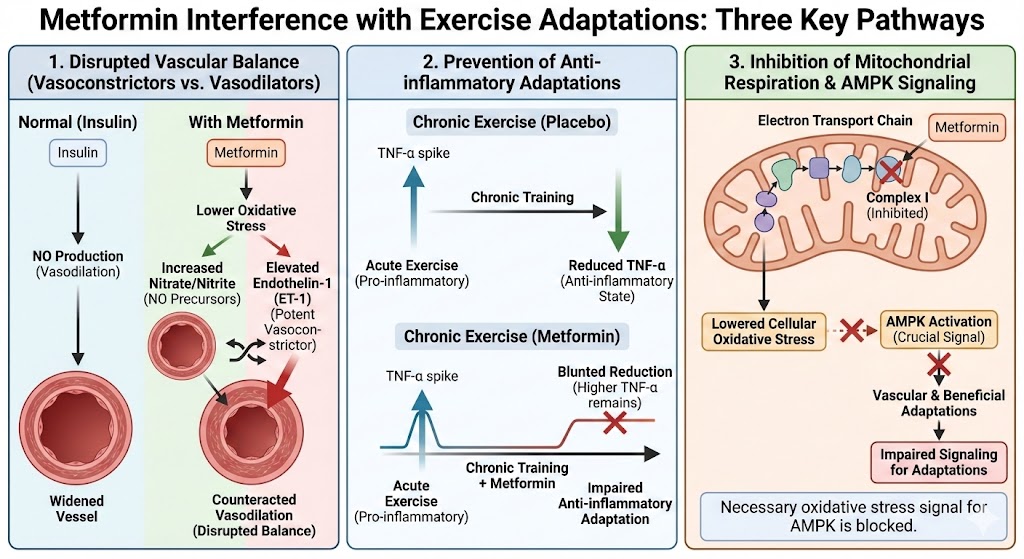
This study hints at three specific biological mechanisms.
The first is a disruption in the balance of vasoconstrictors and vasodilators. Normally, insulin promotes vasodilation (a widening of blood vessels) by stimulating nitric oxide (NO) production. Metformin increased nitrate and nitrite (NO precursors) in this study, but at the same time it caused elevations in endothelin-1 (ET-1), a potent vasoconstrictor that likely counteracted the beneficial effects of NO.
The second is the prevention of anti-inflammatory adaptations. Acutely, exercise is pro-inflammatory, but chronically, it's anti-inflammatory (lowers levels of chronic inflammation). Exercise training with a placebo reduced levels of TNF-α (an inflammatory marker), but exercise with metformin blunted this reduction. In other words, TNF-α levels were higher after exercise with metformin compared to exercise without it.
Third is the inhibition of mitochondrial respiration, specifically at complex I. By doing this, metformin lowers cellular oxidative stress, and while that's often viewed as beneficial, oxidative stress is also a necessary signal (especially during exercise) to active AMPK, which is crucial for signaling vascular and other beneficial adaptations to exercise.
These mechanisms are sufficient to explain the blunted fitness gains and suppressed vascular insulin sensitivity.
|
|
For more on metformin, check out our Metformin topic page, which has information about:
- How metformin impacts the biology of aging
- Metformin's mechanisms and targets
- How metformin affects healthspan and longevity in multiple organisms
- Does metformin lower the risk of age-related diseases in humans?
- Is metformin safe?
- Metformin bioavailability and dosing
- And more!
|
Is Metformin a 'Longevity Drug'?
Enthusiasm for metformin in longevity circles comes from observational data, animal studies, and its mechanistic overlap with pathways known to influence aging.
The initial interest in whether metformin might have benefits beyond glucose control came from a widely cited study in people with diabetes: those taking metformin had about 15% longer survival than non-diabetics (who weren't taking metformin) and 38% longer survival than people with diabetes taking sulphonylureas (another glucose-lowering medication).[1]
There's also the finding that people with diabetes taking metformin have a 31% lower risk of cancer incidence and 34% lower mortality compared to those taking other diabetes drugs.[2] Additionally:
In older adults with diabetes, long-term metformin use is associated with a lower risk of cognitive impairment and dementia.[3] Metformin improves lifespan in worms and has variable effects on lifespan in rodents—low to moderate doses can extend lifespan modestly, but higher doses sometimes shorten it.
However, there are several reasons why I'm cautious of metformin.
An analysis from 2022 called metformin's longevity benefit into question, finding no survival advantage among people with diabetes taking metformin compared to the healthy, general population. In fact, diabetes was associated with up to a 64% increase in mortality risk, even among metformin users.[3]
Although it has a generally good safety profile, metformin interferes with the absorption in vitamin B12 in about 30% of people. This might not lead to a clear deficiency and can be reversed with calcium supplementation, but it's an effect worth mentioning.
The biggest contraindication for metformin for healthy people (and those with diabetes) comes back to exercise. As we've already discussed, metformin dampens some of the most "longevity-relevant" exercise adaptations: better cardiorespiratory fitness and mitochondrial function. This is especially concerning given that VO2 max is a very strong predictor of mortality. Metformin also interferes with resistance training, attenuating gains in lean body mass, muscle mass, and strength.
But the most implicating evidence in my opinion? When put head to head with exercise for preventing diabetes, metformin doesn't even come close. One study I cite frequently is the Diabetes Prevention Program or DPP, which found that just 150 minutes of moderate-intensity exercise per week prevented the progression from prediabetes to diabetes by 58%. Metformin, on the other hand, prevented it by 31%—exercise was nearly twice as effective.
This brings me to a final question. Could all of these negative effects be prevented by altering the timing of metformin or taking it only on non-training days? It's not so straightforward. Metformin's effects (on AMPK and mitochondrial respiration) are chronic, not acute, and even its acute effects last about 36 hours after the last dose. So even if one were to take it several hours away from exercise, the interference is likely to be present.
|
 |
Final thoughts
None of this is medical advice.
If you’re on metformin (especially for diabetes), talk with your doctor before making any changes. For people with type 2 diabetes or very high cardiometabolic risk who struggle to exercise, metformin remains an evidence-based, guideline-supported therapy for improving glycemic control, reducing the risk of complications, and may offer side benefits for cancer and possibly even cognition.
In this context, the drug is doing exactly what it was designed to do.
But for healthy, physically active people, the calculus is different. Any supposed upside for longevity is based on indirect, observational signals and animal data. The downsides, however, include direct trial evidence that metformin blunts key exercise adaptations that likely matter more for long-term health than any small pharmacological effect.
Before reaching for a pill that might slightly touch aging pathways, it makes sense to protect the big, proven lever we already have: robust adaptations to exercise.
For most people, the best "longevity drug" is training hard enough.
|
Warm regards
— Rhonda and the FoundMyFitness team
|
|
|
|
|