 |
Omega-3 supplementation is one of the safest, most evidence-backed ways to support long-term health and longevity.
Today's newsletter will break down a new analysis on the purported link between atrial fibrillation (a dangerous heart arrhythmia) and omega-3s—an area where previous studies have shown concerning associations, but where the research was highly flawed.
Using UK Biobank data, researchers looked at blood omega-3 levels in more than 261,000 adults and followed them for about 12 years. The headline finding was the opposite of what many people have begun to fear—higher circulating omega-3 levels were linked to as much as a 16% lower risk of atrial fibrillation, with a clear dose-response pattern across total omega-3s, DHA, and other omega-3s.
Higher omega-3 levels linked to lower AFib risk
The study—co-authored by Dr. Bill Harris (who was a previous podcast guest) and published in the Journal of the American Heart Association—set out to answer two closely related questions: whether blood omega-3 levels are associated with atrial fibrillation (AFib) risk, and whether self-reported fish oil supplement use is associated with AFib risk—and, if so, whether that relationship is real.
The latter question is relevant, because a study published in 2024 (which I covered in the newsletter and addressed in this clip from a listener Q&A) observed a link between self-reported fish oil use and a greater increase in Afib and stroke risk. This finding generated major headlines and concern among the public.[1]
The problem? This study didn't actually measure omega-3 status in the body, and instead relied on a simple "yes/no" question about supplement use.
In addition to using a more rigorous, biomarker-based analysis, this new study sought to reassess those 2024 findings by using statistical techniques that accurately accounted for age.
To investigate, researchers used UK Biobank data from 261,000+ adults without AFib (average age ~57) with blood omega-3 measurements available, including DHA, total omega-3s, and other omega-3s (ALA, EPA, and DPA) in addition to an expanded cohort of 466,000+ adults who reported whether they used fish oil supplements or not.
Over ~12 years of follow-up, higher circulating omega-3 fatty acid levels were consistently associated with lower AFib incidence. All three omega-3 biomarkers showed clear dose-response relationships: the higher the omega-3 level, the lower the risk.
Here’s what that looked like:
Total omega-3s: Those in the highest category (median 6.3%) had a 14% lower risk of AFib than those in the lowest category (median 2.68%). DHA: The highest levels (median 2.83%) were linked to an 8% lower risk compared to the lowest levels (median 1.24%). Other omega-3s: The highest levels (median 3.65%) were linked to a 16% lower risk compared to the lowest levels (median 1.2%).
One of the most important details was—within the ranges measured—there was no evidence of a U-shaped relationship. Risk reduction generally improved progressively with higher omega-3 levels:
Each ~4% increase in total omega-3s corresponded to an 11% lower AFib risk. Each ~2% increase in DHA corresponded to a 7% lower risk. Each 2.3% increase in other omega-3s corresponded to a 14% lower risk.
|
|
|
You just missed this in your inbox
Every week, Dr. Rhonda Patrick and the FoundMyFitness team distill the latest research into clear, actionable insights on health, longevity, and performance, delivered free to your inbox.
Fish oil use was not associated with AFib risk
In contrast to prior findings, this analysis found no relationship between self-reported fish oil supplement use and AFib risk—no increase, and no decrease.
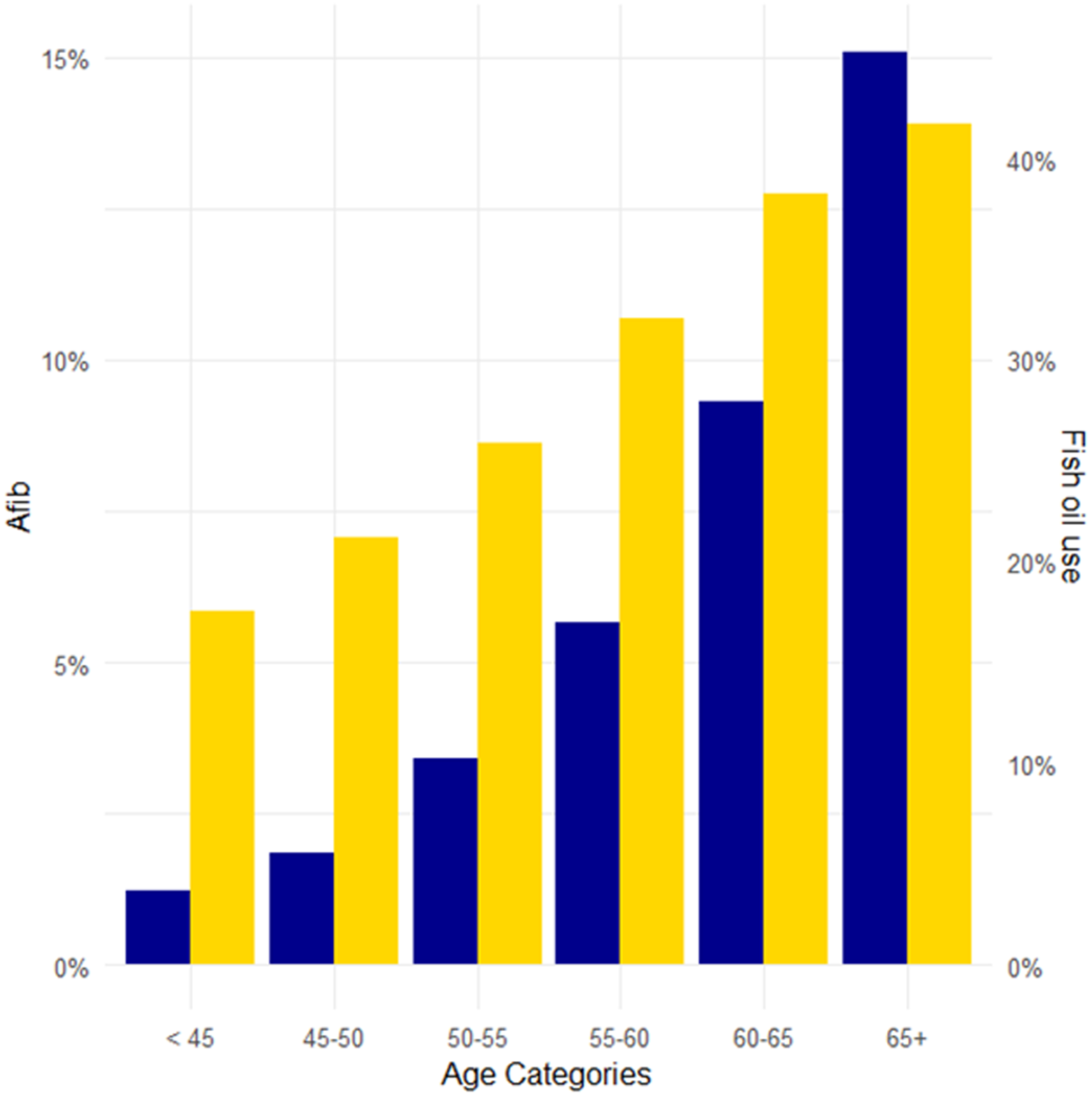
To explain this discrepancy, the authors argue the earlier UK Biobank findings were likely driven by a statistical issue: inadequate adjustment for age. Fish oil supplement users were, on average, older than non-users, and age is one of the strongest predictors of AFib. But the earlier paper adjusted for age using a simple binary cutoff at 65, even though both AFib incidence and fish oil use rise steadily across the lifespan.
When the current study modeled age more appropriately (on a continuous scale or using 5-year increments), the apparent association between fish oil use and AFib disappeared. In other words, once age was handled properly, the “fish oil increases AFib” story fell apart.
Updating the broader evidence base
To place their findings in context, the authors integrated the UK Biobank results with a 2023 meta-analysis of over 55,000 adults. That earlier meta-analysis reported that higher levels of DHA, DHA+EPA, and DPA (but not EPA alone) were linked to lower AFib risk.[2]
With the UK Biobank data added, the overall protective relationship became even clearer: across studies, higher blood omega-3 levels were associated with a 6–10% lower long-term risk of AFib (per quintile increase). The takeaway is consistent across biomarker-based observational evidence—people with higher omega-3 status tend to have a lower risk of developing AFib over time.
|
|
For more on omega-3 fatty acids, check out our Omega-3 topic page, where you'll find information on different forms, the optimal intake for most adults, how omega-3s affect longevity & disease risk, safety and storage issues, and more! |
|
A history of omega-3s and AFib
Decades ago, omega-3 fatty acids garnered attention for being a heart-healthy, anti-arrhythmic nutrient. This was in part due to a landmark Italian study which found that 1 gram per day of fish oil reduced overall mortality, and specifically cut cardiac death in post-heart attack patients by 45%.[3]
Other epidemiological studies at the time reported that consuming fish (baked or broiled but not fried) several times per week was associated with up to a 30% reduction in the risk of AFib.[4] These findings were supported by other smaller randomized controlled studies, such as one from 2005, which gave cardiac bypass patients 2 grams per day of omega-3s, a dose which lowered the rate of post-operative AFib incidence by 54% (relative risk reduction) and reduced the length of their hospital stay.[5] This formed a narrative that omega-3 fatty acids—either from diet or supplements—were likely protective against AFib and overall death from cardiovascular complications.
These generally positive findings were followed up by a few studies that shifted the narrative on omega-3s.
In 2010, a study testing prescription-strength omega-3s (4 grams per day with an initial 8 gram/day loading dose) for 6 months in patients with a history of AFib found no improvement compared to placebo; in fact, there was a non-significant trend for higher AFib recurrence in the omega 3 group.[6] The OPERA study (2012) also found that 2 grams per day of omega-3s did not reduce post-operative AFib incidence compared to a placebo among more than 1,m500 cardiac surgery patients. [7]
Then, in the late 2010s, trials of pharmaceutical-grade, high-dose omega-3 formulations for cardiovascular prevention unexpectedly converged on a concerning signal—higher rates of AFib among patients given omega-3s.
In the STRENGTH trial, AFib incidence was 69% greater among patients given 4 grams per day of EPA+DHA compared to placebo (corn oil).[8] And in REDUCE-IT, 4 grams of pure EPA ethyl ester was associated with a 35% relative increase in AFib, despite major reductions in heart attacks and strokes among the omega-3 group.[9] Furthermore, a smaller trial using 1.8 grams per day of mixed EPA/DHA found a numerically—but not statistically significantly—higher AFib risk (7.2% vs. 4.0%) with fish oil.[10] In contrast, a primary prevention trial in 2021 known as the VITAL-Rhythm study found no significant difference in new AFib cases between fish oil (840 mg/day) and placebo during a 5-year follow-up period.[11]
This string of findings culminated in a meta-analysis of 7 randomized controlled studies, published in October of 2021, which concluded that the use of marine omega-3 fatty acids was associated with a 25% increase in the risk of AFib, which was greater (49% increase) in trials testing doses of more than 1 gram per day but still elevated (12% higher) in studies testing lower doses.[12]
Viewed together, these trials suggested a dose-dependent AFib risk: at very high doses (~4 grams per day), omega-3s are associated with a clear increase in AFib risk; at intermediate doses (~1–2 grams per day), a similar magnitude of risk is observed but with less certainty; and at typical nutritional doses (<1 gram per day), no significant risk emerges. Thus, pharmacological omega-3 supplementation may precipitate AFib, particularly in susceptible individuals or at high doses.
The idea that omega-3s may be pro-arrhythmic was a sharp turnaround from views a decade earlier, but it also sparked debate as to the significance of a 1–2% absolute increase in AFib risk and whether the risk is confined to certain populations. And crucially, it raised an important question: why would fish oil prevent some heart problems but promote arrhythmias in a dose-dependent manner?
|
 |
|
|
Omega-3 fatty acids dosage and risk for atrial fibrillation events in 7 randomized controlled trials based on the meta-analysis by Gencer et al.[12] |
A mechanistic lens
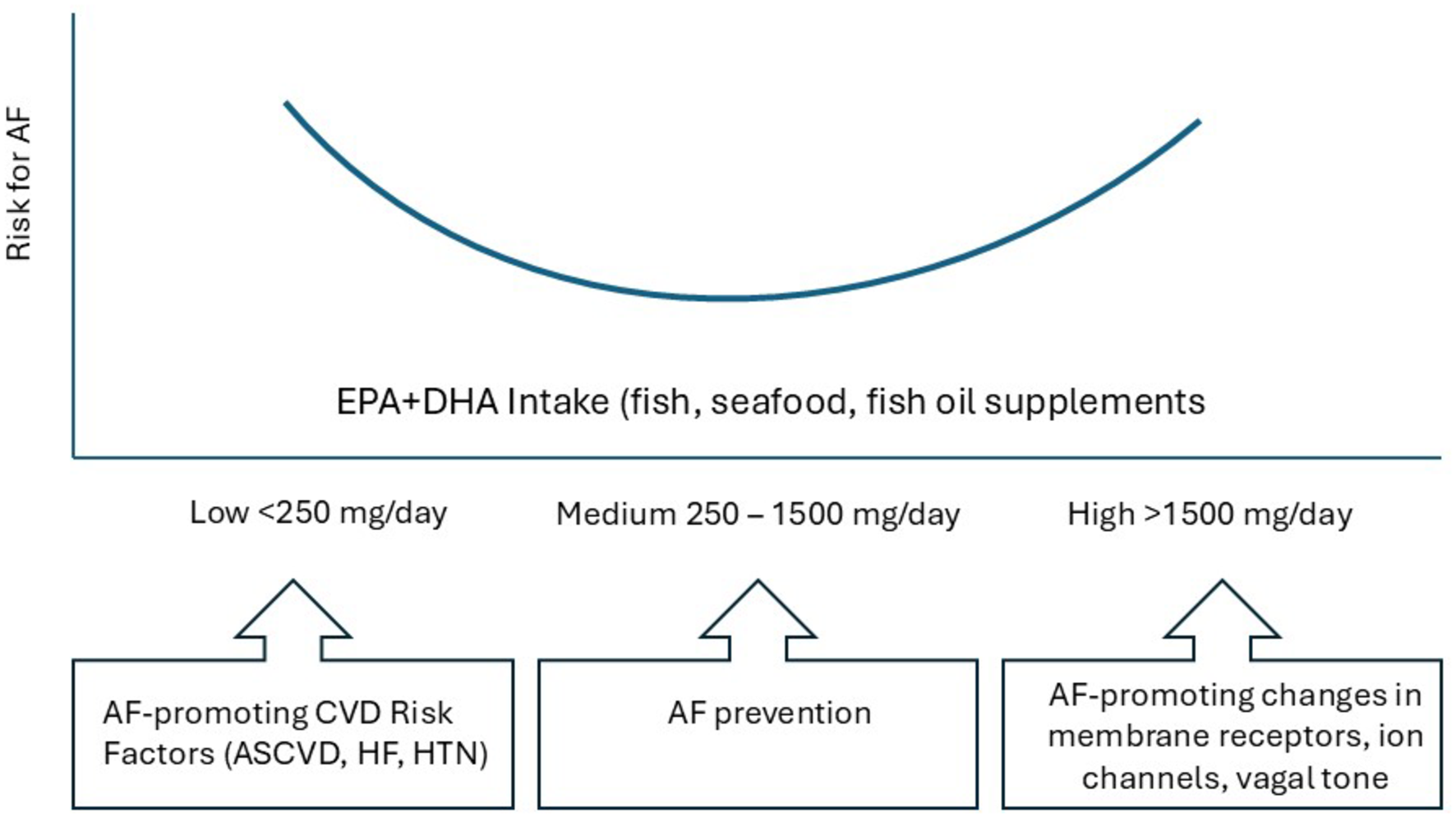
One hypothesis gaining traction—and postulated by Dr. Bill Harris and colleagues—is that omega-3 fatty acids may have biphasic effects on the heart's electrical system: beneficial at dietary doses but deleterious at pharmacologic doses. In other words, a U-shaped relationship.[13]
Exactly how this happens isn't quite understood, but excessive vagal stimulation (parasympathetic activity) is one plausible explanation. Omega-3 intake is known to slow resting heart rate and increase heart rate variability, even causing changes to cell membranes or ion channel function that could promote arrhythmias in susceptible individuals. Mild parasympathetic activity is protective against AFib because it stabilizes electrical activity. And at low to moderate doses, the anti-inflammatory, membrane-stabilizing, and vagal-modulating properties of omega-3s likely confer anti-arrhythmic effects. At higher doses, certain effects like excessive vagal modulation or even pro-arrhythmic changes to the heart's conduction system might promote AFib in susceptible hearts.
This framework neatly explains the dose-response relationships observed: the greatest reductions in AFib risk are seen around an intake of ~650 mg/day of combined EPA+DHA (about 2 servings of oily fish per week or a typical supplement dose), while doses in the 2–4 grams per day range (often given to patients with high triglycerides or cardiovascular diseases) can push individuals into a pro-arrhythmic zone. But the fact that these doses are typically given to patients with diseases should be underscored.
|
|
A pragmatic approach to supplementation
Dr. William "Bill" Harris (a previous podcast guest and one of the world's preeminent experts on omega-3 fatty acids) has been vocal about the current omega-3 and AFib controversy, encouraging a nuanced interpretation of the evidence. In particular, he emphasizes the need to distinguish between physiological omega-3 status (which can be assessed using the omega-3 index) from the act of taking supplements—focusing on what omega-3s are doing in the body rather than assuming that supplements are uniformly harmful or helpful.
His advice is pragmatic: continue eating fish or taking moderate-dose omega-3 supplements, which have multiple cardiovascular benefits, but exercise caution with high-dose omega-3 therapy if you have a history of AFib or are at a uniquely high risk—an approach that aims to maximize the documented benefits of omega-3s while minimizing potential downsides in susceptible people. He and colleagues also stress that Afib itself is manageable and often less life-threatening than the heart attacks or strokes that omega-3s can help prevent.
That doesn't mean we should accept an increased risk as being okay, but that everyone should make a risk-benefit calculation. It's a classic case of personalized medicine—one size does not fit all.
Final thoughts
Zooming in on AFib alone is a bit myopic.
What we really care about is what shifts the needle on lifespan and the big drivers of healthspan—cardiovascular disease, cancer, and overall risk of death. And here the evidence is remarkably consistent: people with higher long-term omega-3 status (best captured by the Omega-3 Index) tend to have lower risk of cardiovascular disease, lower risk of cancer, and lower all-cause mortality. On top of that, omega-3s influence muscle biology in ways that matter as we age, including anabolic and anti-catabolic signaling that may support metabolic health and preservation of lean mass.
I genuinely believe that chronically low seafood-derived omega-3 intake is one of the most underappreciated (and preventable) contributors to disease risk.
In the U.S., most people are sitting below 5% for the Omega-3 Index, while in Japan the average is over 8%... and life expectancy is about five years longer. A practical target is at least 5%, and ideally closer to 8%, because that reflects robust omega-3 status over time.
The good news is that most people can get there.
Two grams per day of EPA+DHA (or more) is typically enough to raise an Omega-3 Index from ~4% to ~8% in about 12 weeks in people who are deficient—which is most Americans. Doing that purely through diet can be hard if you’re not eating seafood nearly every day; for example, you’d need roughly 3–5 six-ounce servings per week of farmed Atlantic salmon to average about 1.5–2 grams per day. For most people, a combination of a few servings of seafood per week plus a quality supplement is the most realistic approach, and it’s what I do.
If you want help choosing the right dose and a high-quality source, I break that down in my free Omega-3 Supplementation Guide—because achieving robust omega-3 status is one of the simplest, most evidence-backed steps you can take for long-term brain health, inflammation resolution, cardiovascular support, and muscle performance.
Don't let media headlines about a single (somewhat limited) study dismiss that.
|
Warm regards
— Rhonda and the FoundMyFitness team
|
|
|
|
|
|