 |
Exercise may not be better than medications or psychological therapy for treating depression… but it’s just as good.
That’s the conclusion of a new meta-analysis, the largest and most rigorous review ever conducted on the effects of exercise for clinical depression.
It found that, compared to no treatment or placebo, exercise had moderate to large effects on reducing depression symptoms, and compared to psychotherapy (e.g., CBT) and antidepressants, there was little to no difference. Exercise wasn't significantly better, but it wasn't worse either.
And while that headline may not seem earth-shattering on the surface, it’s actually incredibly profound.
Because it suggests one of our most well-studied longevity and healthspan interventions is also a clinically powerful tool for treating a condition that affects about 332 million people worldwide—roughly 4% of the world's population. Yet despite how common depression is, movement is often the missing piece: two thirds of people with major depressive disorder don't meet basic physical activity guidelines, and when researchers measure activity objectively rather than relying on self-report, that shortfall is even larger.
This gap between what we know works for both mind and body—and what people are actually able to do in the real world—is where this research becomes so important.
Today we’re unpacking what this meta-analysis tells us, and what it means for how we think about exercise as medicine.
|
|
|
The study was a Cochrane review—Cochrane tends to be the gold standard for evidence synthesis—and it was an update of a review originally published years ago. Importantly, this update added a substantial number of new randomized controlled trials, ultimately including 69 studies (at least 4,985 participants) in the meta-analysis.
This review also wasn’t about “movement” in a general sense. It specifically focused on exercise, defined as planned, structured, repetitive bodily movement intended to improve or maintain fitness, with interventions lasting at least one week. In other words, these findings speak to exercise training, not just physical activity broadly (other interventions, such as sauna, have shown meaningful benefits for depression, as I discuss with Dr. Ashley Mason on episode #67 of the FoundMyFitness podcast).
A major strength of the review is that it handled many of the real-world complexities that make exercise research messy—but also clinically relevant. For example, the authors:
Classified exercise intensity (very light, light, moderate, vigorous, and near maximum) using American College of Sports Medicine (ACSM) criteria. Used data from the largest exercise dose when trials included multiple dose arms, while also running a sensitivity analysis using the lower-dose arms. Included only each study’s primary depression outcome measure when multiple depression scales were reported.
You just missed this in your inbox
Every week, Dr. Rhonda Patrick and the FoundMyFitness team distill the latest research into clear, actionable insights on health, longevity, and performance, delivered free to your inbox.
How did exercise compare with standard treatments?
The central question was straightforward: How does exercise compare to (1) control conditions (no treatment/usual care) and (2) psychotherapy or antidepressant medications for reducing depressive symptoms?
Exercise vs. no treatment/control
Across 57 trials, exercise produced a moderate-to-large reduction in depressive symptoms. However, the authors rated the certainty of this evidence as low, largely because many trials had methodological weaknesses (more on that below). Notably, even when the analysis used the lowest exercise dose (instead of the largest-dose arm), exercise still showed a moderate benefit versus control.
Exercise vs. psychotherapy and antidepressants
This is the comparison most people care about—and it’s where the evidence is thinner. These head-to-head comparisons included far fewer participants than the exercise vs. control trials.
Compared to psychotherapy (10 studies, 414 participants), exercise was essentially equivalent, indicating little to no difference between approaches. Compared to antidepressant medications (5 studies, 330 participants), exercise was also similarly effective.
|
|
 |
(In this clip, Dr. Charles Raison explains how agents that interact with the immune system may play a subtle and complex role in depression). |
What about long-term follow-up?
This is where the literature is still frustratingly limited. For exercise vs. control, results at follow-up (ranging from 8 weeks to 12 months) continued to favor exercise, but the certainty was low due to limited data and high variability between studies. Follow-up comparisons versus psychotherapy or medication also suggested similar effectiveness over time, but again, evidence certainty was low.
Does the “type” of exercise matter?
“Exercise” is a big umbrella term, so the practical question is whether how you do it changes how effective it is. The review explored this using subgroup analyses. These are useful for generating clues about what might matter most, but they’re not the same as trials that directly randomize people to different exercise “prescriptions,” so the conclusions here should be read as directional, not definitive.
Number of sessions (dose over time)
When the authors grouped trials by the total number of exercise sessions, here's what they found:
0–12 sessions: moderately effective 13–36 sessions: largely effective ≥37 sessions: moderately to largely effective
This pattern suggests that meaningful benefits can occur even with relatively fewer sessions, but the largest average effect appeared in the mid-range (13–36 sessions), roughly the difference between brief exposure and a sustained, structured program. Importantly, differences between these subgroups were not statistically significant, so this should be interpreted as a trend.
Exercise intensity
Across very light, light, moderate, and vigorous intensity categories, effects consistently favored exercise, with moderate-to-large effects across the board. Subgroup differences weren’t statistically significant.
In practical terms, this suggests that depression-related benefits of exercise are not confined to a single “optimal” intensity zone, which is encouraging from an adherence and accessibility standpoint (I dive deep into the brain benefits of vigorous exercise in this solo episode).
Type of exercise
Aerobic, resistance, and combined training all favored exercise. Estimated effects were:
Aerobic: moderately to largely effective Resistance: largely effective Combined (aerobic + resistance): largely effective, and more effective than either aerobic or resistance exercise in isolation.
Combined programs showed the largest average effects, which makes intuitive sense—they often deliver a broader physiological stimulus and more structured engagement. Still, some of these subgroups included fewer studies, so differences in the sizes of the effect may also reflect differences in study design, supervision, or participant characteristics. But it does fit with our general knowledge that a well-rounded exercise program usually beats out doing a single type of exercise in isolation, no matter your intended outcome.
The control condition matters more than most people realize
One final analysis looked at what exercise was being compared to, and this turned out to be critical. Effects were largest when exercise was compared to no treatment, waitlist, usual care, or self-monitoring—situations where the comparison group received little structured engagement.
When exercise was compared to a placebo-like control, however, estimated benefits were smaller and far more uncertain, suggesting that part of exercise’s apparent benefit reflects non-specific effects that could be due to expectations, attention, social interaction, routine, and the act of committing to a structured intervention.
|
 |
Where the evidence is limited (and why certainty was downgraded)
A major reason the authors rated much of the evidence as "low certainty" comes down to a fundamental challenge in behavioral interventions (especially those involving exercise): blinding.
Unlike drug trials, exercise can’t be masked. Participants know whether they’re exercising, and researchers often do as well. This opens the door to performance bias, where expectations shape outcomes. In depression research, where symptom measures are inherently subjective and often self-reported, beliefs about what “should” work can meaningfully influence results. This helps explain why exercise often looks more effective compared to no treatment than when compared to placebo or active controls.
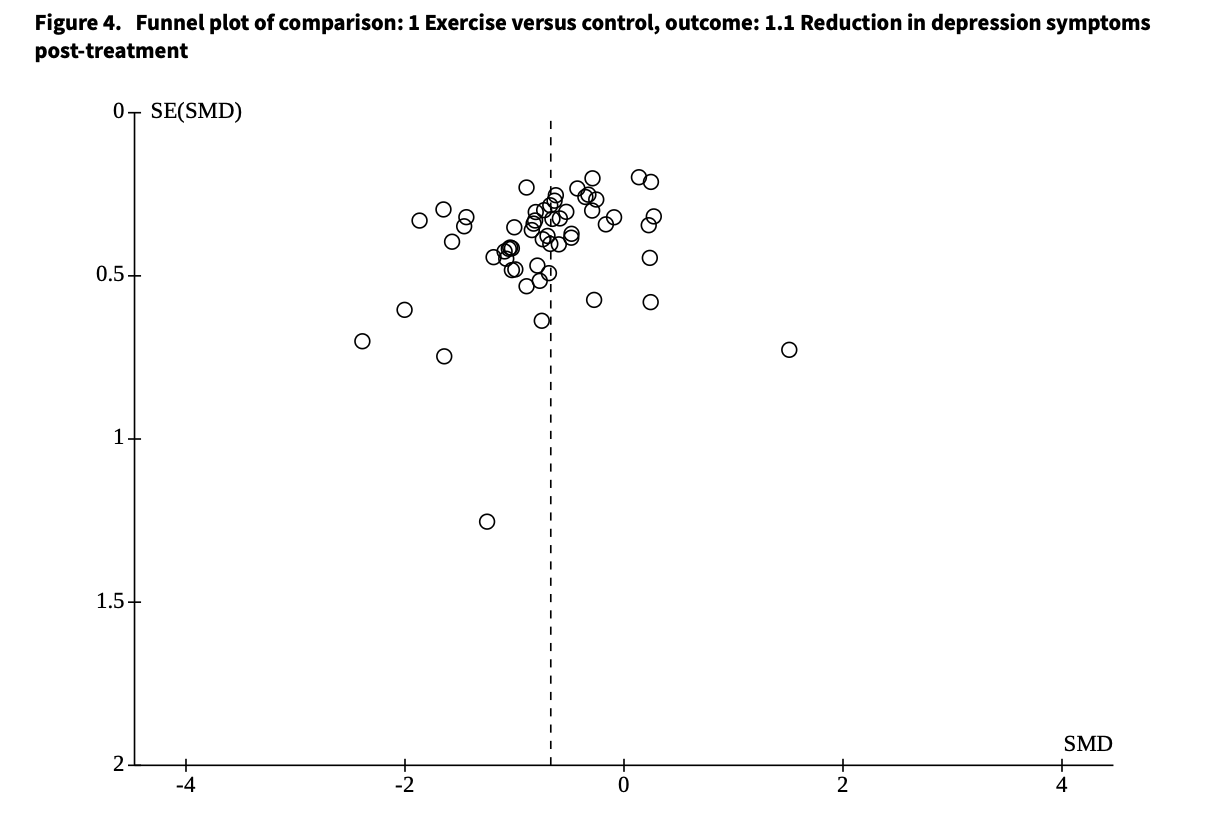
Another important limitation is publication bias. This is the tendency for positive studies to be published more often than null ones. The authors found evidence consistent with this bias and estimated that 15 studies may be "missing" from the published literature. After accounting for these, the estimated benefit of exercise dropped but was still meaningful.
Final thoughts
For clinical depression, the evidence still isn’t airtight enough to say exercise should be recommended as a standalone treatment for everyone. But as an adjunct therapy, it’s hard to argue against it.
For patients who can tolerate it (and with appropriate medical oversight when needed), exercise should be close to a default prescription. And for those without clinical depression who are looking for a temporary mood boost or cognitive performance bump, the benefits of exercise are undisputed.
Even if this new review slightly tempers the most sensational headlines, there’s a genuinely positive way to interpret what it found. When you account for the built-in challenges of exercise trials like no true participant blinding, publication bias, and limited long-term follow-up, the signal doesn’t disappear. It shrinks. After stress testing the evidence from multiple angles, a meaningful, moderate benefit still remains.
So, exercise still moves the needle for people with clinical depression, and unlike most other treatments, it also improves cardiometabolic health, physical function, and long-term disease risk, all without the side effects common to many medications.
A therapy that can support mental health while simultaneously strengthening the foundations of healthspan is rare. “Not better, but just as good” is far from underwhelming in this case—it reinforces that everyone should see movement as central to mental health.
|
Warm regards
— Rhonda and the FoundMyFitness team
|
|
|
|
|
|