 |
Intermittent fasting is no more effective for weight loss than standard dietary advice.
That’s the conclusion of a new meta-analysis on fasting, and a lot of people are sharing it as proof that “intermittent fasting has no benefits.”
I don’t think that’s what it shows.
What it does show is pretty straightforward. In controlled trials (where calories are matched), IF produced weight loss similar to standard dietary advice, and generally better than doing nothing. That’s exactly what you’d predict if the driver is energy intake.
But for many people, fasting is a simpler, more sustainable way to achieve a calorie deficit than counting calories.
And weight loss is hardly the only reason that people fast intermittently.
There’s evidence that fasting can influence glucose regulation, circadian biology, sleep, and as we will see today, cognitive function. A study led by Dr. Mark Mattson (a previous podcast guest), found that fasting led to superior improvements in a few specific measures of cognitive function and a unique metabolic fasting physiology that a "healthy diet" did not.
This fasting physiology is created by a mild energy deficit that flips a “metabolic switch” in the body. And it helps explain fasting’s unique cognitive benefits.
|
 |
You just missed this in your inbox
Every week, Dr. Rhonda Patrick and the FoundMyFitness team distill the latest research into clear, actionable insights on health, longevity, and performance, delivered free to your inbox.
IF’s cognitive benefits
When it comes to the brain health benefits of fasting, the intermittent metabolic stress may be far more important than the specific fasting schedule.
In this regard, fasting's biggest real-world strength is that it can quietly generate an energy deficit—a repeated, intermittent metabolic challenge. Because the brain is exquisitely sensitive to the body's metabolic state, especially in aging and insulin resistance, fasting could provide unique benefits for cognition and brain aging.
That's where a centerpiece study by Dr. Mark Mattson and colleagues comes in.
The 8-week study randomized older adults with insulin resistance to either:
5:2 intermittent fasting (two consecutive “fasting” days per week, using two meal-replacement shakes totaling 480 calories per day), or a Healthy Living diet implemented every day.
To track cognition, they measured executive function with a test battery (yielding an overall executive composite plus domain factors derived from multiple tasks), and also assessed verbal and logical memory with some standard neuropsychological tests.
Two features make this paper especially relevant to our theme of why an energetic stress is central to some of IF’s benefits.
The first is that IF clearly produced a larger energy deficit. When the researchers estimated average daily intake, calories fell by roughly 28% in the IF group vs. 13% in the healthy diet group, a meaningful separation in net energy balance over the 8-week intervention.
Second, the fasting group showed the physiologic signature of fasting. Ketone bodies—β-hydroxybutyrate (BHB) and acetoacetate (AcAc)—rose in the IF group, but not in the healthy diet group, confirming that the fasting protocol pushed participants into a distinct metabolic state.
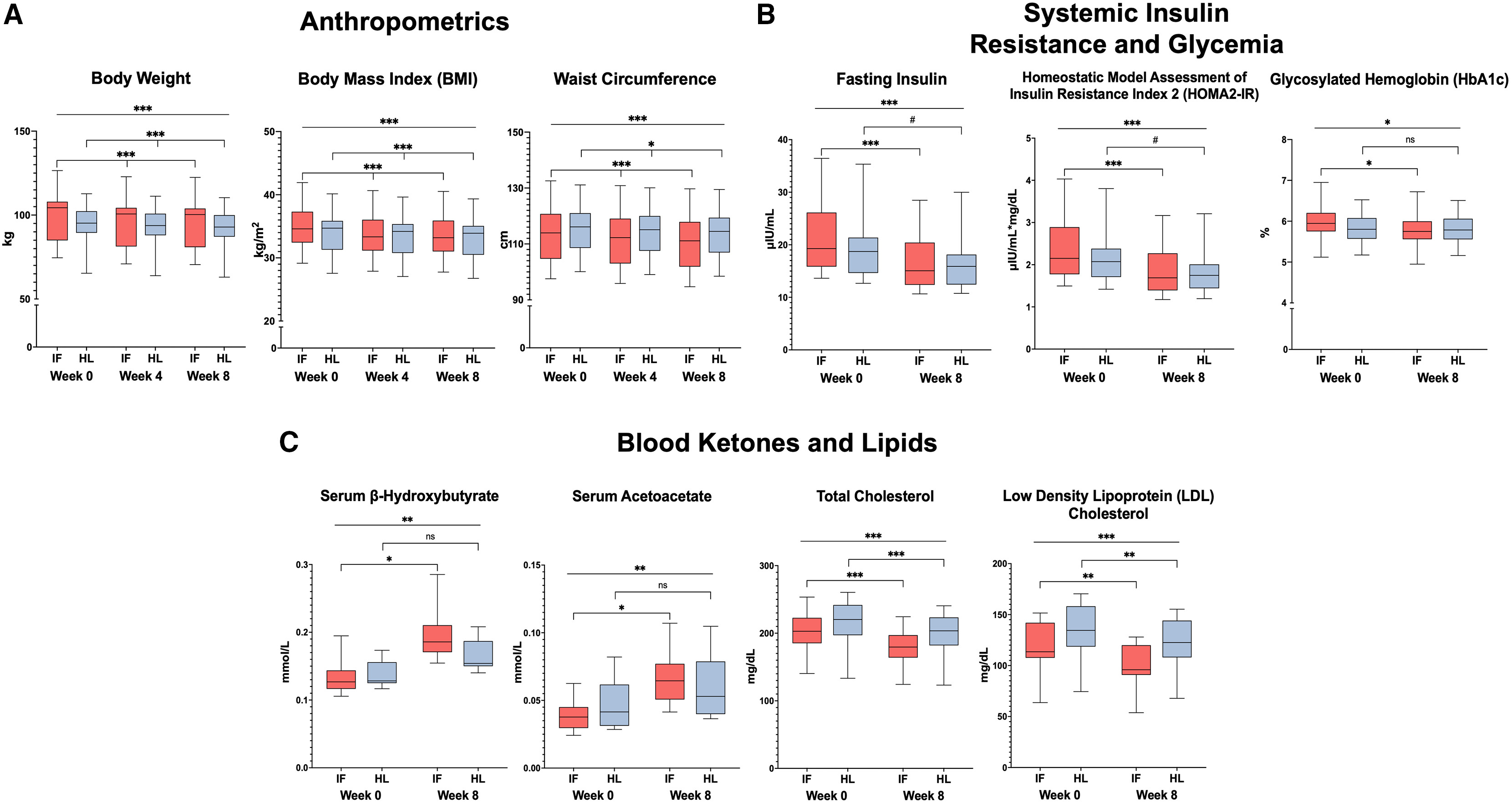
Both groups improved on anthropometric and metabolic measures over the intervention. IF was more effective for overall body mass and BMI, consistent with the larger energy deficit, but the two diets were broadly similar in several cardiometabolic outcomes, including changes in waist circumference and systemic markers like insulin resistance, HbA1c, and blood lipids (all improved to a similar degree after IF and the healthy diet).
|
|
Changes in body composition, insulin resistance/glucose measures, and blood ketones and lipids during the study. |
Brain physiology improved on both diets
Both diets produced meaningful changes in brain-related physiology. Across groups, the interventions:
reduced neuronal insulin resistance, lowered brain glucose, and slowed the pace of brain aging (BrainAGE) by about ~2.5 years on average over the 8-week period.
However, Alzheimer’s disease biomarkers did not change (a finding the authors describe as "sobering"). Amyloid markers (Aβ42, Aβ40) and p181-tau remained essentially unchanged after either diet.
|
In my most recent member Q&A, I address several questions related to fasting and autophagy, including:
- Does prioritizing protein conflict with fasting for autophagy?
- Does autophagy happen during sleep?
- What are the effects of "cheat meals" on autophagy and fasting's benefits?
- What do you think about ProLon's fasting-mimicking diet?
Listen to member Q&A #78 with Dr. Rhonda Patrick
|
Executive function favors fasting
The paper gets compelling when we zoom in on cognitive function.
Some executive function outcomes improved in both groups, but IF separated itself from the healthy diet in the more demanding, higher-order components of executive control.
-
The executive function composite score and a domain known as the fluency factor improved within the fasting group but not within the healthy diet group (although the between-group comparison trended in the same direction, it didn't meet conventional thresholds for statistical significance).
But the clearest separators were specific executive processes tied tightly to prefrontal control—strategic planning and cognitive flexibility (switching between demanding task sets). Both improved in the intermittent fasting group but not in the healthy diet group.
Memory outcomes showed a more mixed picture.
- There were shared gains across both diets in several measures, including immediate recall, short-delay free recall, and both short- and long-delay cued recall.
-
IF edged ahead on short-delay cued recall (remembering recently learned information after a brief break, with a hint to jog your memory) and a was more noticeably advantageous for long-delay cued recall (remembering that same information, just later, after enough time has passed that it's no longer "fresh").
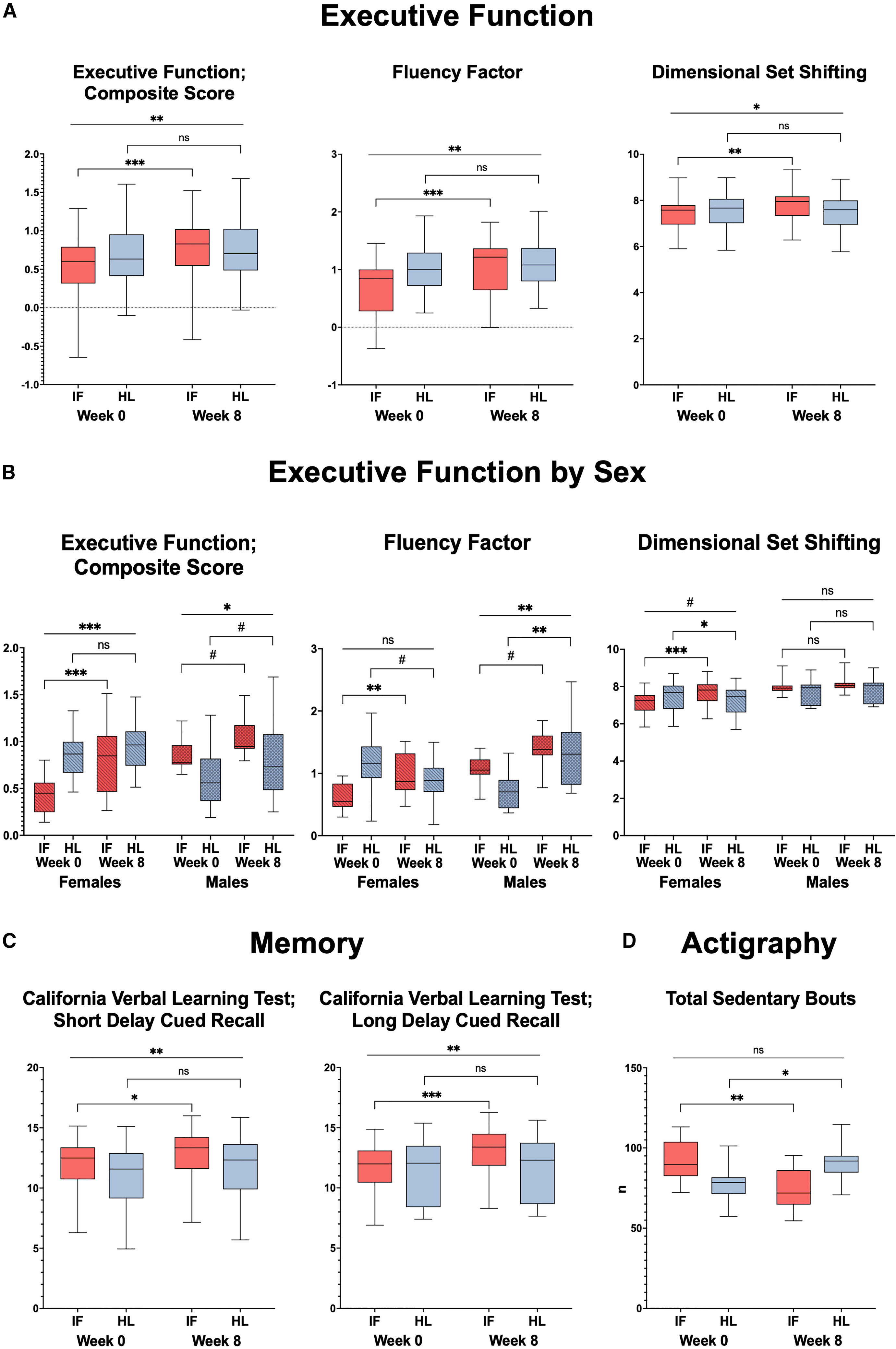
Last is a finding that is interesting and frankly, quite surprising. The fasting advantage for executive function appeared more obvious in women, who showed a significant improvement in executive function with IF but not with the healthy diet, whereas men tended to improve with both interventions, making the effects look less diet-specific in men.
This is hard to explain mechanistically from this single study and should be treated as exploratory. It’s not evidence that fasting helps women and not men, but it is a signal that might reflect baseline differences, adherence, metabolic responsiveness, or simply small-sample variability.
|
|
Cognitive function outcomes and physical activity levels. |
Flipping the metabolic switch
The reason why fasting and the mild, intermittent energy deficit it creates are so beneficial to the brain and body is that it flips a "metabolic switch" in our body.
As humans, we evolved to thrive in both fed and fasted states, and this led to the development of so-called "metabolic flexibility"—the ability to switch between carbohydrates (carbs) and fats as a source of energy for our muscles and brain.
After we eat, our body uses carbohydrates (glucose) as an immediate source of energy. And if we haven't eaten for a few hours, our body will use stored glucose (glycogen) as an energy source. But if we've fasted for a while—say 12–36 hours or more—or engaged in prolonged or vigorous exercise, the body transitions from using glucose and glycogen to mobilizing fat stores and producing ketone bodies.
That's the metabolic switch.
Remarkably, the metabolic switching and ketosis induced by fasting create a biochemical environment that is potentially neuroprotective, providing the brain with an efficient and "clean" fuel source in the form of ketone bodies and activating pathways for neuron growth, repair, and stress resistance.
Ketones provide the brain with an efficient fuel source. They readily cross the blood-brain barrier, and neurons use them efficiently as an energy source (and with less oxidative byproducts than glucose burning). But ketones aren't just energy, they're signaling molecules that activate anti-inflammatory and antioxidant genes that help the brain function optimally even without food. They upregulate brain-derived neurotrophic factor (BDNF) which supports neuron growth, connectivity, and resilience. And they trigger cellular stress-response pathways that promote the body and brain's cellular cleanup process called autophagy.
These mechanisms have been demonstrated in animal and human studies, and they're strong evidence that the mental clarity and focus people report while fasting aren't just anecdotal, they're real, and driven by the intermittent metabolic switching and cellular stress response of ketones, BDNF, and autophagy that's hardwired into our biology.
|
 |
Final thoughts
The "magic" of fasting isn’t that we can’t explain its benefits or mechanisms, but its ability to facilitate a mild energy deficit more easily, and more sustainability, compared to other forms of dietary restriction (like counting calories).
Tracking when you eat tends to be a much easier lever than meticulously tracking what you eat (though both can be effective).
It's unfortunate that IF has gotten a bad reputation in recent years, with claims that you'll lose muscle mass and strength while doing it or that it's a poor tool for weight loss or weight management, when in fact it's perfectly compatible with both of these goals.
IF can work for building muscle mass and strength in the gym… as long as you're eating adequate calories and protein to support growth. And it’s also effective for weight loss if it helps you to eat fewer calories by restricting when you eat.
Many people, including myself, find massive benefits with IF/time-restricted eating, including improved morning energy and better sleep at night (early-day eating matches insulin sensitivity while late-day eating disrupts glucose and sleep). The metabolic health benefits, circadian alignment aspect (when done right), and brain/hormesis mechanisms are all also well-supported by the literature.
Of course, fasting can have downsides. Fasted training and narrow eating windows can compromise energy availability and sap training volume, energy, and short-term performance. Overly restrictive dieting can also lead to micronutrient deficiencies, mood disturbances, and hormone disruption. But none of these are consequences of fasting per se, but rather a chronic nutrient deficiency.
I hope it's clear by now that I don't stand firmly on either side of the "fasting is good" or "fasting is bad" debate. It's context dependent.
And that's why when you see headlines that "intermittent fasting doesn't work," you need to ask "for what?" Because the answer to that is probably more important than the conclusion of a single study or meta-analysis.
|
Warm regards
— Rhonda and the FoundMyFitness team
|
|
|
|
|