 |
Your sleep tonight depends on what you eat today.
A new analysis paired food logs with at-home sleep tracking to see which dietary shifts actually change how long we sleep and how restful that sleep is.
On higher-fiber, more plant-diverse days, people logged more deep and REM sleep, less light and fragmented sleep, and had a lower overnight heart rate. On days with more processed foods, saturated fat, and animal-based foods, nighttime wakefulness was higher and they had a "less restorative" sleep stage distribution.
And when dinner made up a larger share of daily calories, people slept longer with a higher overnight heart rate. Meanwhile, a longer interval between one's last meal and bed time was associated with slightly less sleep and a lower overnight heart rate.
Today’s newsletter breaks down why the within-person design of this study is a big upgrade over what's typically done in observational studies on diet and sleep, and what it suggests about the foods (and timing patterns) most likely to help your sleep tonight. It may be less about protein, fat, and carbs and more about food quality and when you concentrate calories across the day.
Today's diet affects tonight's sleep
Most diet–sleep studies ask the blunt (and less-informative) question of whether people who eat better sleep better. The problem is that people who eat better also tend to differ in a thousand other ways that affect sleep like their stress, routines, health status, chronotype, socioeconomic factors, and more. So it’s hard to know whether diet is doing the work or whether diet is just a marker for a whole lifestyle package.
This new study comes at the question from a different angle. Instead of comparing, say, a higher fiber eater to a lower fiber eater, it leans heavily on dietary variation within the same person. It asks whether what a person ate yesterday can predict how they'll sleep that night.
In other words: on the days you eat differently, does your sleep change in a detectable way?
Researchers used data from 3,598 adults from the Human Phenotype Project, a longitudinal digital health study that paired time-stamped dietary logs with clinically validated in-home sleep testing that captured total sleep time, sleep staging (deep/REM/light), continuity (efficiency, time to fall asleep, nightly awakenings), and even average sleeping heart rate (a useful window into overnight autonomic tone).
This still isn’t a randomized trial, so it can’t prove causation with absolute certainty, but it’s closer than most observational nutrition work (the authors refer to it as "quasi-causal") for a few reasons. For one, it naturally controls for stable traits like genetics, personality, baseline health, and chronotype by comparing people to themselves across different days. It also gets the time order right by modeling how today's diet affects tonight's sleep while adjusting for the prior day's diet and sleep. This helps reduce reverse causation (because poor sleep can change how you eat the next day).
Meal timing mostly influences sleep duration
Meal timing didn't drastically reshape sleep stages… it mostly showed up in how long people slept and how “revved up” their bodies stayed overnight.
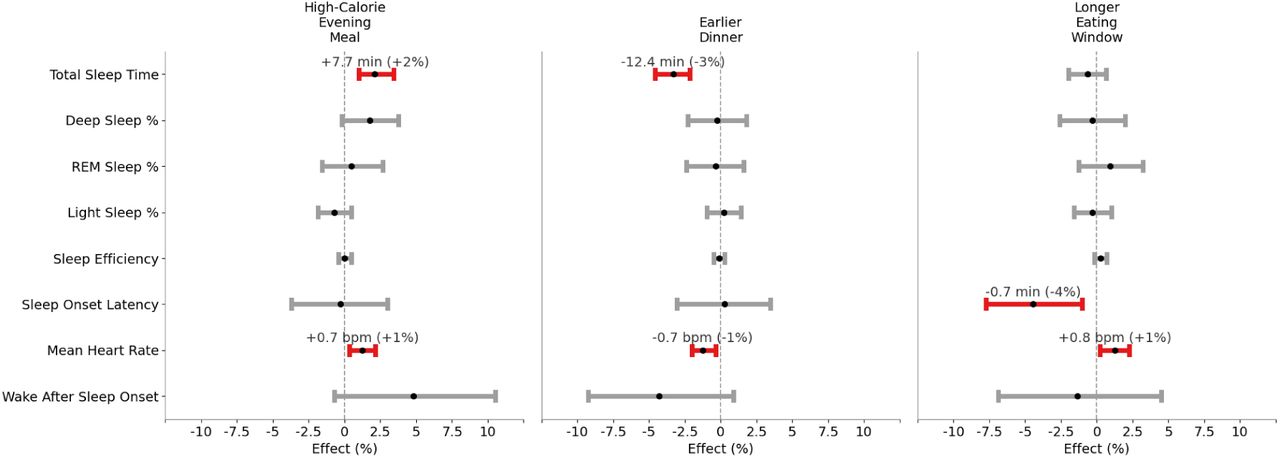
Earlier dinner timing (last meal 4 hours before bed vs. ~2 hours before bed) was linked to about 12 minutes less total sleep, but also about a 1 bpm lower sleeping heart rate. A higher-calorie evening meal (dinner with 46% of total daily energy versus 29%) was linked to about 8 minutes more total sleep, but also about a 1 bpm higher sleeping heart rate. A longer daily eating window (12.7 hours versus 9.6 hours) tended to track with about a 1 bpm higher sleeping heart rate and a 4.5% shorter time to fall asleep.
|
|
The effect of meal timing on sleep. |
You just missed this in your inbox
Every week, Dr. Rhonda Patrick and the FoundMyFitness team distill the latest research into clear, actionable insights on health, longevity, and performance, delivered free to your inbox.
Diet composition shifts sleep stages
What really moved sleep stages was diet composition and quality.
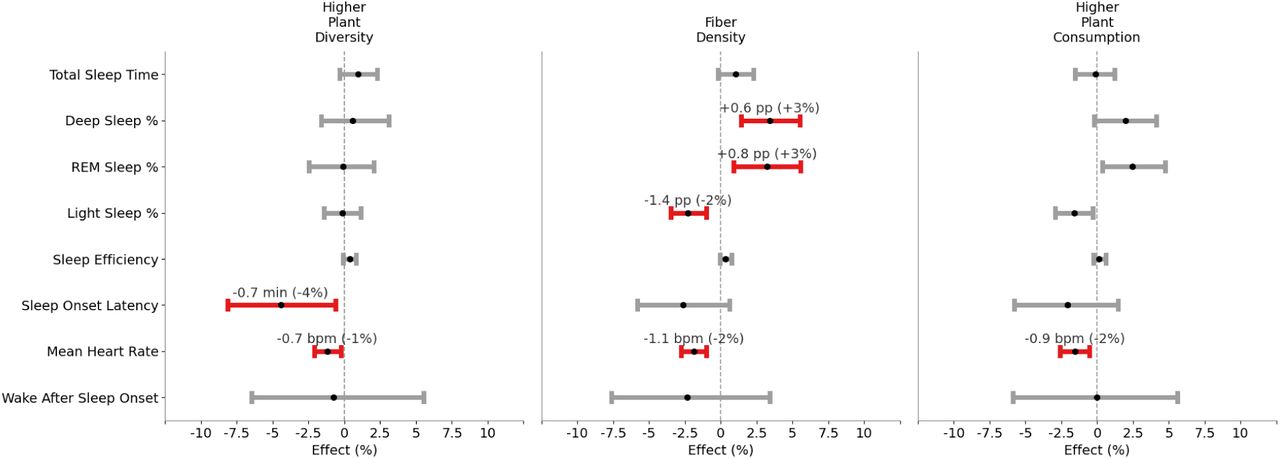
Higher fiber density (15.7 grams of fiber/1,000 calories vs. 9 grams/1,000 calories) was associated with a 1 bpm lower sleeping heart rate, plus a redistribution of sleep stages in a more “restorative” direction including more deep sleep and REM sleep, and less light sleep. Greater plant diversity (7 vs. 3 unique plant-based food items per day) was linked to a small improvement in sleep onset latency (falling asleep a bit faster) and a lower overnight heart rate. A higher plant consumption (as a percentage of total daily calories) was also associated with a 1 bpm lower overnight heart rate.
|
|
The effect of diet composition on sleep. |
A few micronutrients show consistent effects
Most micronutrients didn’t show short-term effects, but a cluster of plant-associated micronutrients showed directionally consistent trends toward more deep/REM sleep, and in some cases lower overnight heart rate and a longer sleep duration.
Magnesium (485 vs. 249 mg/day) trended toward more deep sleep and more REM sleep. Vitamin C (154 vs. 58 mg/day) trended toward more deep sleep, more REM sleep, and longer total sleep time. Folate/folic acid (468 vs. 261 mg/day) trended toward more deep and REM sleep, and a lower nighttime heart rate. Vitamin E (12.4 vs. 6.7 mg/day) trended toward more deep and REM sleep, and greater total sleep time.
In contrast, macronutrient distribution—one's percent of calories from protein vs. carbs vs. fat—showed no short-term effects on sleep physiology.
That doesn’t mean macronutrients never matter, but it suggests that in the real world, night-to-night sleep changes may be more sensitive to food quality and timing than to shifting macro ratios by modest amounts.
The paper did note some broader food source patterns, like more whole-food/plant-forward days aligning with more deep/REM sleep and less fragmented sleep, and more processed food and saturated fat aligning with more nighttime wakefulness and less deep/REM sleep.
|
|
|
The effects of specific micronutrients on sleep. |
| |
|
In member Q&A #72, I do a deep dive into what causes fragmented sleep and which strategies, nutrients, and supplements I recommend to improve sleep depth and continuity. I cover:
-
What causes nighttime awakenings—insomnia, sleep apnea, and frequent nighttime urination
- Does excessive fluid intake at night disrupt sleep?
- The effect of psychological stress on sleep disruption
- Irregular sleep schedules, alcohol, late-night eating, caffeine, blue light, and aging
- Sleep-promoting strategies—morning bright light exposure, bedtime routines, and bedroom temperature
- Melatonin, magnesium, L-theanine, glycine, and myo-inositol
Watch Q&A #72 with Dr. Rhonda Patrick
|
|
Why fiber promotes sleep
Long-time listeners will know that I love mechanism—the science that explains how things like diet and exercise improve our health. That's why I had to dive deeper into this fiber–sleep relationship. Why might fiber and plant-forward eating patterns translate into better sleep that same night?
One plausible explanation is that fiber feeds gut microbes that convert fermentable carbohydrates into short-chain fatty acids or SCFAs. When you look at the research (albeit mostly in rodents), SCFAs turn out to be not just metabolic byproducts, but bioactive sleep signals. In one study, elevating levels of the SCFA butyrate using a pro-drug led to a nearly 50% increase in non-REM sleep and also reduced body temperature, implicating butyrate as a bacterial-derived sleep-promoting signal.1
SCFAs also seem capable of influencing sleep through multiple gut–brain pathways. For example, microbes can increase serotonin production in the gut by using SCFAs to upregulate the rate-limiting enzyme for serotonin production known as TPH1. And while gut serotonin isn't identical to brain serotonin, this is still important for downstream gut–brain communication and melatonin biology. SCFAs can also act as cues for the circadian clock by entraining intestinal circadian rhythms through an HDAC-inhibiting mechanism. They may therefore stabilize timing signals that coordinate metabolism, gut function, and circadian biology… all of which feed back into sleep regulation.
The gut microbiota also produce other metabolites that influence sleep, including serotonin, melatonin, tryptophan, and GABA—dietary timing, composition, and regularity influence gut microbiome composition and thus influence the production of these gut-derived metabolites.
There are even some interesting echoes of this mechanistic story in humans.
Controlled feeding studies have shown that higher fiber intake is associated with more slow-wave sleep (saturated fat showed the opposite association).2 A greater daytime intake of fruits and vegetables (and other "healthy" carbohydrates) was linked to less disrupted sleep the same night—a 5-cup increase in fruit and vegetable intake was associated with a 16% improvement in sleep quality.3 Supplementing with a prebiotic (yeast mannan) led to more non-REM sleep and a greater time in bed compared to a placebo, effects attributed to changes in the SCFA propionate and the inhibitory neurotransmitter GABA.4
|
 |
Final thoughts
We often focus on light exposure, screens, or temperature for sleep hygiene, but this study nudges us to expand that conversation. What we eat, just like when we eat, is part of the equation. If you’re doing everything else right but still struggling with sleep, think of food as another piece of the puzzle.
From my own experience, meal timing has been huge. I aim for my last meal about three hours before bed, and I’ve seen it lower my overnight heart rate. Plus, people track this on wearables and notice the difference too (lots of comments on my recent X post confirmed that!)
Now, while I haven’t done a deep dive on exactly which foods impact my sleep, eating more whole, clean foods (especially plants loaded with phytochemicals and micronutrients) seems to support better sleep. It likely ties back to better glucose regulation and the sleep-supporting nutrients we’ve touched on. It’s a neat feedback loop!
So, do I think everyone needs to stop eating three hours before bed? Not at all! Some people might benefit from protein closer to bedtime or something to curb hunger. But the research does suggest that if you want to experiment with better sleep, these tactics are worth trying.
Lean into a more plant-forward and fiber-rich diet during the day, maybe include those plants in a lighter evening meal—perhaps making that last meal around 25% of your daily intake rather than half.
It’s all about finding what works best for you. But it's nice to have research to help inform strategies (and support a mechanism too).
|
Warm regards
— Rhonda and the FoundMyFitness team
|
|
|
|
|
|