 |
Ever wonder why some carbs spike your blood sugar more than others? New research shows that your metabolic health defines your personal "carb-response type."
Researchers gave healthy adults seven different meals (rice, bread, potatoes, pasta, beans, berries, and grapes) and tracked their blood sugar responses.
The highest blood glucose response differed greatly between individuals:
• 35% were “rice-spikers” (they experienced their highest glucose response after eating rice)
• 24% were “bread-spikers”
• 22% were “grape-spikers”
Crucially, one's unique metabolic health (especially insulin sensitivity) predicted their blood sugar response. Insulin-resistant individuals had dramatically higher blood sugar responses to potatoes and pasta compared to insulin-sensitive individuals, who tended to spike the highest with rice and grapes. Eating protein, fiber, or fat before carbs helped insulin-sensitive people significantly reduce glucose spikes but barely helped insulin-resistant people.
These results are a friendly reminder that individual biology, not just carb type or glycemic index, determines how your body responds to food.
It's a compelling case for personalized nutrition.
You just missed this in your inbox
Every week, Dr. Rhonda Patrick and the FoundMyFitness team distill the latest research into clear, actionable insights on health, longevity, and performance, delivered free to your inbox.
What's Your "Carb-Response Type"?
To determine the influence of metabolic physiology and other molecular features on post-meal glucose responses, researchers conducted a continuous glucose monitoring study involving 55 men and women without diabetes.
Each participant underwent a detailed assessment of their metabolic health, including measures of whole-body, liver, and fat-cell insulin resistance, beta-cell function, cardiometabolic risk factors, and comprehensive analyses of their microbiome, metabolome, lipidome, and proteome. Think of these "-omes" as different maps of the body's internal landscape: the metabolome tracks small chemical compounds, the lipidome studies fats, and the proteome focuses on proteins. Each provides unique insights into metabolic function.
Participants consumed seven standardized meals designed to test their postprandial glycemic response—essentially, how much their blood glucose spiked after eating. Each meal contained exactly 50 grams of carbohydrates but varied in carb type and fiber content. The seven meals included:
- White rice
- Buttermilk bread
- Cooked and cooled potatoes
- Cooked and cooled pasta
- Canned black beans
- Mixed berries (strawberries, blueberries, blackberries)
- Grapes
These meals represented diverse carbohydrate profiles, ranging from low-fiber starches (rice and bread), high resistant-starch carbs (potatoes and pasta), high-fiber starches (black beans), and both low- (grapes) and high-fiber (berries) simple sugars.
Participants also tested three "mitigators" before eating white rice: a fiber source (pea fiber), a protein source (egg whites), and a fat source (cream), to evaluate their effectiveness in reducing glucose spikes. Ten grams of each of the mitigators was consumed 10 minutes before the participants ate rice (the most glucose-elevating carb source).
Beware of Potatoes and Pasta—If You're Insulin Resistant
Rice caused the highest glucose spike overall, with 35% of participants identified as "rice-spikers." Another 24% spiked highest with bread, and 22% with grapes—unsurprising, given their lower fiber content. No participant spiked highest after eating high-fiber meals (black beans or berries).
Yet, glucose responses varied significantly depending on participants' insulin resistance and beta-cell function. Insulin-resistant individuals experienced dramatically higher glucose spikes from potatoes (179% higher) and pasta (152% higher) compared to insulin-sensitive participants—even though these foods contained slowly digesting starches.
Conversely, insulin-sensitive individuals spiked most from rice and grapes but had lower glucose responses after potatoes and pasta. In fact, glucose responses to grapes were similar between insulin-sensitive and insulin-resistance participants, while the responses to potatoes were not. This led researchers to coin a term: the potato to grape ratio (PG-ratio)—it's a measure of how much one's glucose spikes after eating potatoes compared to grapes. A higher ratio means a greater glucose spike after potatoes; insulin-resistant individuals had a much higher PG-ratio than insulin-sensitive individuals.
|
|
|
Blood glucose responses to each meal among the different "carb-response types." |
 |
| |
Want to learn the best ways to control blood glucose? I took a deep-dive into some strategies in Premium Member Q&A #61.
-
19:51 - What's the best way to lower your glucose levels?
-
21:07 - Why muscle matters for glucose control
-
22:36 - Why do refined carbs cause glucose spikes?
-
25:32 - Can eating carbs last prevent glucose spikes?
-
27:00 - Two supplements clinically shown to reduce HbA1c
-
30:27 - How much sleep is optimal for glucose regulation?
-
31:55 - Do cinnamon and apple cider vinegar really lower blood sugar?
|
|
| |
Mitigating Glucose Spikes with Protein, Fiber, and Fat
Consuming any of the "mitigators" (protein, fiber, and fat) significantly reduced glucose spikes, with fiber most effective, followed by protein and fat. Fiber reduced peak glucose by 11 mg/dL, protein by 10 mg/dL, and fat by 8 mg/dL compared to rice alone. All mitigators slightly delayed peak glucose time and lowered glucose area-under-the-curve (AUC), though not significantly.
However, responses to these mitigators varied widely based on individual metabolic profiles. Insulin-resistant participants saw little or no benefit from any mitigator. In contrast, insulin-sensitive individuals experienced substantial reductions, particularly from fiber (a 28 mg/dL reduction vs. just 7 mg/dL in insulin-resistant individuals). Protein and fat also reduced glucose spikes in insulin-sensitive participants (by 22 mg/dL and 11 mg/dL, respectively). Protein, but not the other mitigators, showed the biggest benefit to participants who were "rice-spikers."
Does this mean that eating protein, fiber, or fat before a high-carb meal won't lead to a lower glucose spike? Not at all—this strategy works for many people.
What it does mean is that we shouldn't automatically assume everyone will experience a benefit from, say, eating protein before a carb-heavy meal. It's important to tailor dietary strategies based on individual metabolic responses and "food sensitivities."
If rice (or grapes or potatoes, or pasta) are your "weak spot," metabolically speaking, it might be prudent to eat some protein, fiber, or fat along with that meal if you're concerned about a glucose spike.
|
|
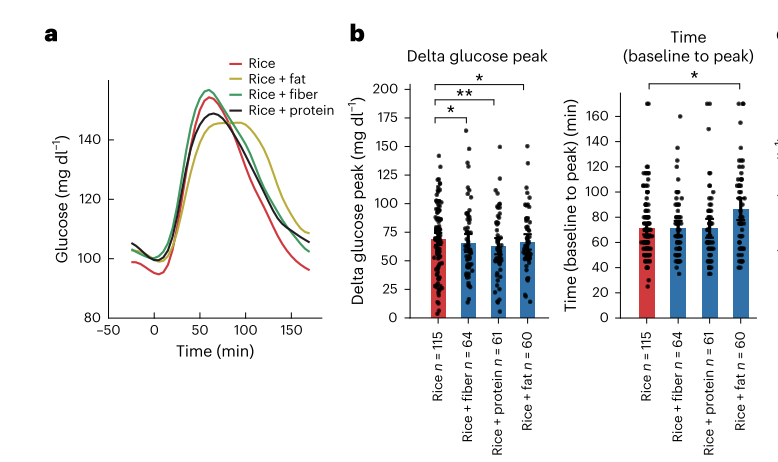 |
Postprandial blood glucose responses to each meal among the different "carb-response types." |
Hidden Factors Behind Your Carb Response
Another intriguing aspect of this study was its exploration of the hidden molecular and microbiome features associated with each person's unique blood sugar responses and metabolic health. The researchers identified several key markers—molecules, lipids (fats), proteins, and specific types of gut bacteria—that were strongly linked to how participants responded to different carbohydrate-rich foods. For instance:
- "Bread-spikers" had elevated levels of a specific metabolite called N1-Methyladenosine, which has previously been linked to high blood pressure. Interestingly, these bread-spikers also had higher overall blood pressure, potentially increasing their risk for cardiovascular disease.
-
"Potato-spikers" had notably higher levels of triglycerides and fatty acids circulating in their blood, consistent with their increased insulin resistance. Their blood also showed elevated levels of proteins involved in liver fibroblast activation pathways which are linked to liver dysfunction or fatty liver disease.
Molecular markers were grouped into two main clusters, reflecting either healthy or compromised metabolic states. Insulin resistance was associated with higher levels of certain metabolites, such as tyrosine, hydroxybutyric acid, and glutamic acid, along with triglycerides, fasting insulin, BMI, and free fatty acids. Specific gut bacteria genera like Slackia and Tyzzerella were also more abundant in insulin-resistant participants.
On the other hand, insulin-sensitive individuals had lower levels of molecules such as phosphatidylcholine, lysophosphatidylcholine, and threonic acid. They also showed higher levels of certain beneficial gut bacteria, including Butyrivibrio, Asaccharobacter, and Fusicatenibacter. One analysis suggested that pathways in the beneficial gut bacteria Bacteroides thetaiotaomicron positively mediated liver insulin resistance and fasting insulin.
Some microbiome features even influenced how effectively protein, fiber, or fat could reduce blood sugar spikes from carbohydrate meals. For example, higher levels of some bacteria appeared beneficial, enhancing the blood-sugar-lowering effects of pre-meal protein, fiber, or fat. Additionally, specific enzymes produced by gut bacteria were associated with higher blood sugar responses, possibly indicating issues like insufficient dietary fiber intake.
Overall, these findings highlight that beneath a seemingly simple measure like blood sugar control lie complex molecular and microbial interactions. Understanding these hidden factors provides a valuable window into personalized approaches to improving metabolic health…at least once the science can inform us of strategies to modify these factors.
|
|
|
Final thoughts
These findings aren’t just interesting, they fundamentally challenge traditional nutritional guidelines. Instead of generalizing that some carbs are universally "good" or "bad," it's clear that individual metabolic physiology dictates glucose responses more accurately than carbohydrate type alone. What's important here is not which sources spiked glucose the most or by how much—but rather, the incredible variability in responses among the participants.
This study also underscores the limitations of the glycemic index (GI), a common measure ranking carbs based on their blood-glucose-raising potential. According to these findings, GI is virtually meaningless for predicting an individual's actual blood glucose response, which is far better predicted by insulin sensitivity, beta-cell function, and a host of other molecular features. Furthermore, one's response to a food with the same GI might change daily, depending on sleep, exercise, or what foods it's combined with.
Personal experience confirms this: I've talked many times about how I learned I was uniquely sensitive to grapes after wearing a CGM for a few weeks—I'm a "grape-spiker."
Nutrition truly is personal. Understanding your unique "carb-response type" may involve experimenting with tools like continuous glucose monitors or carefully observing mood and weight fluctuations post-meal.
Whether you're a "rice-spiker," a "grape-spiker," or something entirely different, your metabolic health journey is unique—and your nutrition strategy should be too.
|
Hi all! Rhonda here. I recently appeared on two fantastic podcasts, and I'd love for you to check them out:
On The Diary of a CEO, I talked about:
- Why I increased my creatine dose from 5 grams to 10 grams daily
- Infrared saunas versus traditional saunas
- Practical steps you can take today to reduce your risk of cognitive decline
On The Tim Ferriss Show, we discussed:
- The supplements I recommend to my own parents
- My updated perspective on fasting and alcohol consumption
- A surprising recent study showing that glass bottles contain more microplastics than plastic bottles
I hope you enjoy these conversations as much as I did! Talk to you next week.
Rhonda 💜
|
|
|
|
|
|