 |
Alzheimer’s research has long been framed as “amyloid vs. tau.” But a new study points to a third player—a trace element measured in micrograms—that may be just as central. Lithium appears to function as part of the brain’s built‑in defense system; when amyloid‑β plaques trap and sequester it, that defense falters.
In mouse models, dialing down lithium by about half triggered changes that look like the earliest stages of Alzheimer’s Disease: more amyloid deposition, more tau phosphorylation, inflammation, and a loss of synapses and myelin. Restoring lithium, using a lithium-elevating salt at low, physiologic doses, both prevented and reversed pathology.
This isn’t the first hint that lithium matters in brain aging, but it’s the most comprehensive case yet that lithium homeostasis could be pivotal in the onset and trajectory of Alzheimer’s disease.
In today’s email, we’ll unpack what the study actually did, why an enzyme known as GSK3β sits at the center of the story, and what these findings might mean for protecting the aging brain.
You just missed this in your inbox
Every week, Dr. Rhonda Patrick and the FoundMyFitness team distill the latest research into clear, actionable insights on health, longevity, and performance, delivered free to your inbox.
Lithium Deficiency is a Driver of Alzheimer's Disease
For the study, researchers investigated 27 abundant and trace minerals in the brain and blood of (postmortem) brain of people with mild cognitive impairment and Alzheimer's disease or adults with no cognitive impairment (the controls).
Of all of the metals analyzed, lithium was the only one consistently reduced in people with mild cognitive impairment—a clinical state often preceding Alzheimer's disease. The prefrontal cortex or PFC, a hub of memory and executive function, showed the steepest decline, while the cerebellum (a region known to be relatively spared in Alzheimer's disease) was unaffected.
The reason for lithium deficiency was clear. Amyloid-beta plaques appear to act as "molecular sponges" for lithium; they trap it inside insoluble deposits. Plaques from affected brains were enriched in lithium, and the degree of lithium sequestered in the plaques increased as disease progressed. The result was a functional lithium deficiency in the surrounding cortex, and importantly, the lower the cortical lithium levels, the worse a person’s cognitive test scores.
|
|
|
| |
In mice, reducing cortical lithium by about half—accomplished by feeding them a lithium-deficient diet—was enough to drive Alzheimer’s-like pathology, including:
- an accelerated deposition of amyloid-beta proteins and phosphorylated tau.
- the activation of microglia (the brain's immune cells) into a more pro-inflammatory state.
- a loss of synapses, axons, and myelin sheaths
-
faster cognitive decline.
Lithium-deficient mice, whether they were predisposed to develop Alzheimer's disease or not, had several neurological and behavioral characteristics consistent with the disease.
At the genetic level, lithium deficiency produced changes overlapping with those seen in neurodegenerative disease. Alzheimer's risk genes (including Apoe) and inflammatory and neurodegeneration pathways were upregulated while genes involved in synaptic signaling, myelin production, and amyloid clearance were downregulated.
The result is a vicious cycle: less lithium, more amyloid, weaker clearance, and more inflammation. Exactly the kind of cascade we'd expect to lead to Alzheimer's disease.
|
|
|
|
GSK3β as a Central Switch
One of lithium’s best-known molecular targets is glycogen synthase kinase 3 beta (GSK3β), an enzyme long implicated in Alzheimer's disease pathology. In this study, lithium deficiency tipped the balance toward hyperactive GSK3β, increasing the total amount of the protein while simultaneously elevating levels of its active form and reducing its inhibitory form.
This hyperactivation drove tau phosphorylation, microglial cytokine release, and a loss of myelin proteins. Blocking GSK3β reversed many of these lithium-deficiency–induced changes. In other words, lithium may act as a natural brake on GSK3β, and without it, the kinase runs wild.
Lithium Therapy Reverses Alzheimer's Disease Pathology
If lithium deficiency contributes to Alzheimer's, why not just give lithium back? It seems like a simple solution, but the challenge is that traditional lithium salts, like lithium carbonate, also get taken up into amyloid plaques, limiting their bioavailability.
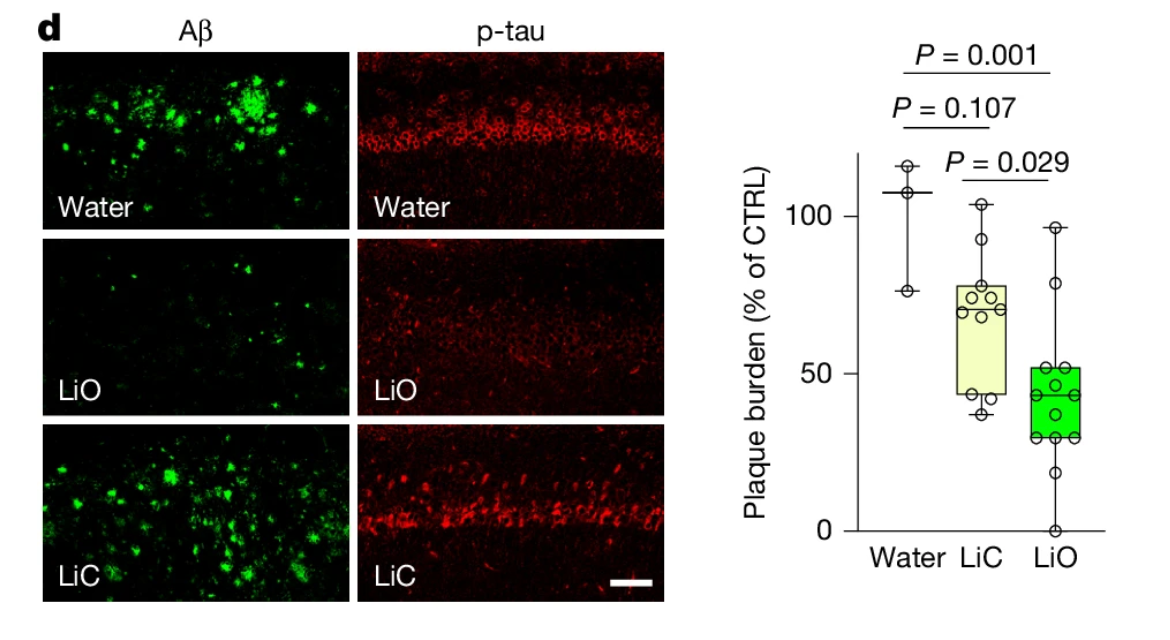
In a search for novel lithium salts, the researchers identified lithium orotate (LiO) as a smarter alternative. Unlike lithium carbonate, LiO didn't bind as readily to amyloid proteins, meaning more lithium stayed available in the “free” cortical tissue. That's exactly what was observed in the Alzheimer's disease mouse models. LiO almost completely blocked amyloid plaque deposition and tau phosphorylation, reducing pathology in mice with advanced disease—cognitive performance improved in both Alzheimer's mice and normal aging mice, with a near-complete reversal of memory deficits. Perhaps most importantly, low-dose LiO was non-toxic. Long-term administration did not disrupt kidney or thyroid markers—common concerns with conventional lithium therapy.
This is all great, but what are the human implications? The research also addressed that, though briefly. In a cohort of normally aging humans, cortical lithium levels positively correlated with working memory and performance on a cognitive test known as the Mini-Mental State Exam or MMSE. Early but not definitive evidence that what was shown in mice may also occur in humans.
This work reframes lithium as a physiological micronutrient for brain resilience. Much like iron deficiency drives anemia, lithium deficiency may accelerate neurodegeneration. While the leap from mice to humans is large and clinical trials are needed, a low-dose, amyloid-evading supplement like lithium orotate could one day help preserve cognition during aging.
(If you’re looking for more information, I do a deep dive on low‑dose lithium for dementia prevention in Q&A episode #69 and discuss why I don’t supplement with lithium for neuroprotection in Q&A episode #56.)
|
|
| |
Q&A Episode #69 covers Rhonda's thoughts on lithium in the context of dementia prevention
- What is the history of lithium for neuropsychiatric conditions?
- How does lithium work in the brain?
- Is lithium associated with lower rates of dementia and Alzheimer's disease?
- What do randomized controlled trials show regarding lithium supplementation and Alzheimer's disease in neuropsychiatric patients?
- Does lithium supplementation improve cognitive function in people with dementia and Alzheimer's disease?
- Which form of lithium supplementation is most effective?
- Is lithium supplementation safe?
- Does Rhonda supplement with low-dose lithium?
|
|
Does the Evidence Support Low-Dose Lithium for Dementia Prevention?
The idea that simply restoring lithium—strategically, in the right form—could interrupt the cascade of Alzheimer’s disease is both elegant and profound. That said, we should be careful not to jump to the conclusion that lithium supplementation will be broadly beneficial for all brain‑related conditions.
Lithium is best known as a prescription mood stabilizer for bipolar disorder. That history matters because lithium has a narrow therapeutic window—the distance between an effective dose and a toxic one is small. That's why we should be cautious about using lithium outside of medical supervision, especially in the context of over‑the‑counter supplements where people may “mega‑dose," even if accidentally. It’s not a nutrient that should be taken liberally.
Ecological and observational work has reported intriguing associations between trace lithium in drinking water and a variety of outcomes—fewer psychiatric hospitalizations, lower aggression and suicide rates, reduced mortality from cardiovascular disease and Alzheimer’s disease, and even lower prevalence of type 2 diabetes and obesity. But these are correlations. When controlling for factors like obesity, diabetes, and inactivity, the apparent protection against Alzheimer’s disappears. It's not convincing evidence.
More formally, a 2024 meta‑analysis of seven observational studies found that people prescribed lithium (typically for bipolar disorder) had a ~41% lower risk of Alzheimer’s disease and ~34% lower risk of all‑cause dementia than non‑users. That’s encouraging, but it’s also indirect: these participants weren't taking lithium to prevent dementia, which limits how cleanly we can generalize to the broader population.[1]
On randomized trials, the picture is mixed. A systematic review of 13 RCTs plus three non‑randomized trials—mostly in neuropsychiatric cohorts—found that roughly half of studies showed a clear benefit of low‑dose lithium for slowing cognitive decline in Alzheimer’s disease or as an adjunct in depression/mania. Study designs varied and many had limitations, so again, we should be hesitant to over‑interpret these results for dementia prevention per se.[2]
The most promise is seen in trials involving mild cognitive impairment.
- Over 12 months, low‑dose lithium stabilized cognition versus placebo and reduced Alzheimer’s biomarkers, including phosphorylated tau.
- In a two‑year, double‑blind follow‑up, the placebo group declined while the lithium group remained stable, with better memory and attention at 24 months. At 36 months, the lithium group showed higher CSF Aβ42, consistent with less brain amyloid deposition.
For people already diagnosed with Alzheimer’s disease, results vary, but there are bright spots: in one study (~113 participants), a microdose (300 µg/day) of lithium prevented cognitive decline over 15 months, whereas the placebo group deteriorated. A small meta‑analysis of three clinical trials with a total of 232 participants supports a modest slowing of cognitive decline in AD/MCI with lithium.[3][4][5]
Finally, formulations matter. Lithium carbonate is the prescription standard and the form used in most human trials. However, lithium orotate is an over‑the‑counter supplement sometimes promoted as crossing the blood–brain barrier more readily, theoretically allowing lower doses. That remains speculative: we don’t have large, head‑to‑head human trials comparing lithium orotate and carbonate, and we don’t know whether easier membrane crossing could also increase uptake into kidneys or thyroid, raising long‑term safety concerns. But as this study shows, this form also appears to evade uptake by amyloid beta proteins, making it more bioavailable to the brain.
Nonetheless, the absence of robust safety data—especially with the possibility of people taking high doses—should give us pause.
Final thoughts
At this point, I see low-dose lithium as intriguing but not yet prescriptive. The evidence, particularly in mild cognitive impairment, points to some stabilization of cognition and improvements in Alzheimer’s biomarkers, but there are still too many unanswered questions about optimal dosing, duration of use, which populations are most likely to benefit, and which formulations are safest. For people who are intent on experimenting, I would strongly emphasize the importance of doing so under medical supervision. If it were to be considered at all, it should be in the form of a very low “microdose” in the microgram range, rather than the milligram doses used in psychiatric treatment, and it should be accompanied by monitoring of safety labs such as serum lithium, kidney function, and thyroid function.
There's also a mild contraindication for pregnant women. Lithium crosses the placenta and may cause mild birth defects. It can also increase the risk of preterm birth. So, it's usually avoided to start it during pregnancy. If a woman is already using lithium before pregnancy for things like a severe bipolar disorder, it’s not an absolute contraindication as long as the benefits still outweigh the risks.
As for me, I’m not supplementing with lithium for neuroprotection right now. Instead, I’m focusing on omega-3 fatty acids, which also affect membrane biology and have a much stronger safety profile. Lithium is already part of most people’s daily intake, even without supplements. Trace amounts occur naturally in drinking water—with levels varying widely by region—and in foods grown in lithium-rich soil, including vegetables (like potatoes, beets, spinach, and cabbage), legumes, whole grains, and to a lesser extent in dairy and animal products. Typical diets provide 0.2–1 mg per day, far below psychiatric doses but possibly enough to support normal brain physiology.
That said, I am following the lithium research closely, especially the studies that are beginning to explore dose, duration, and the comparative safety of different lithium salts. I find the emerging data encouraging, but until we know more—particularly about lithium orotate and its long-term safety—lithium for dementia prevention remains, in my view, an experiment that belongs in carefully controlled clinical trials or under direct medical guidance.
|
|
|
|
Warm regards
— Rhonda and the FoundMyFitness team
|
|
|
|
|
|