 |
Obesity is far more than a metabolic disorder. It dramatically accelerates cognitive decline.
Being overweight or obese has been linked to dementia risk for decades, and now new genetic data shows a causal link.
For every 5-point increase in body mass index, there's a 63% increase in dementia risk, plausibly driven by vascular damage linked to chronically elevated blood pressure.
Indeed, high blood pressure emerged as the critical mediator, explaining roughly one-quarter of this obesity-dementia connection. While metabolic dysfunction, including elevated blood glucose, cholesterol, and inflammation, is independently associated with dementia risk, these factors did not prominently mediate the specific obesity-driven pathway in this analysis.
The findings strongly emphasize that maintaining a healthy weight and controlling blood pressure are key strategies for preserving cognitive function and reducing dementia risk.
|
|
|
What makes this new study different is that, instead of stopping at correlations, the authors set out to test the much harder claim of whether a higher body mass index, or BMI, (a common measure calculated from height and weight to estimate body fatness) causally increases the risk of vascular-related dementia (which they defined as vascular dementia + “unspecified” dementia), because “unspecified” dementia tends to share vascular/cardiometabolic risk factors and because obesity shares so many risk factors with cardiovascular disease, especially hypertension.
And they designed the study to address the two big reasons observational findings in this space often contradict each other: confounding and reverse causation.
If you simply compare people with higher versus lower BMI, you immediately run into confounding (BMI tracks with everything from diet to physical activity, to smoking history to medication use, to access to healthcare). Dementia adds an extra twist; because it has a long preclinical phase, people can start losing weight years before diagnosis. That can distort the data so dramatically that you end up with the familiar U-shaped curve, where both low BMI and high BMI look risky, even if low BMI isn’t truly causal.
So the authors used Mendelian randomization or MR, which is essentially using genetics as a “natural randomized controlled experiment,” to ask whether people who inherit genetic variants that predispose them to higher BMI also have a higher risk of vascular-related dementia. If yes, that’s evidence the relationship is more likely causal and not just an artifact of lifestyle confounding or preclinical weight loss (we'll discuss these later on).
The researchers tackled the question from multiple angles—each one addressing a different weakness of the others:
They first looked at the association between BMI and vascular-related dementia risk in three big datasets:
Copenhagen City Heart Study and the Copenhagen General Population Study (126,655 adults) UK Biobank (377,755 adults)
Next, they used MR to reduce confounding and reverse causation. Here’s how to think about it: Some people inherit genetic variants that nudge BMI slightly higher across life. Others inherit variants that nudge BMI slightly lower. If higher genetically predicted BMI also predicts higher vascular-related dementia risk, that supports a causal interpretation.
This rests on three key assumptions that the variants:
genuinely influence BMI. aren’t systematically tied to lifestyle/environmental factors that independently affect dementia risk. influence dementia risk through BMI, not through unrelated biological pathways.
|
|
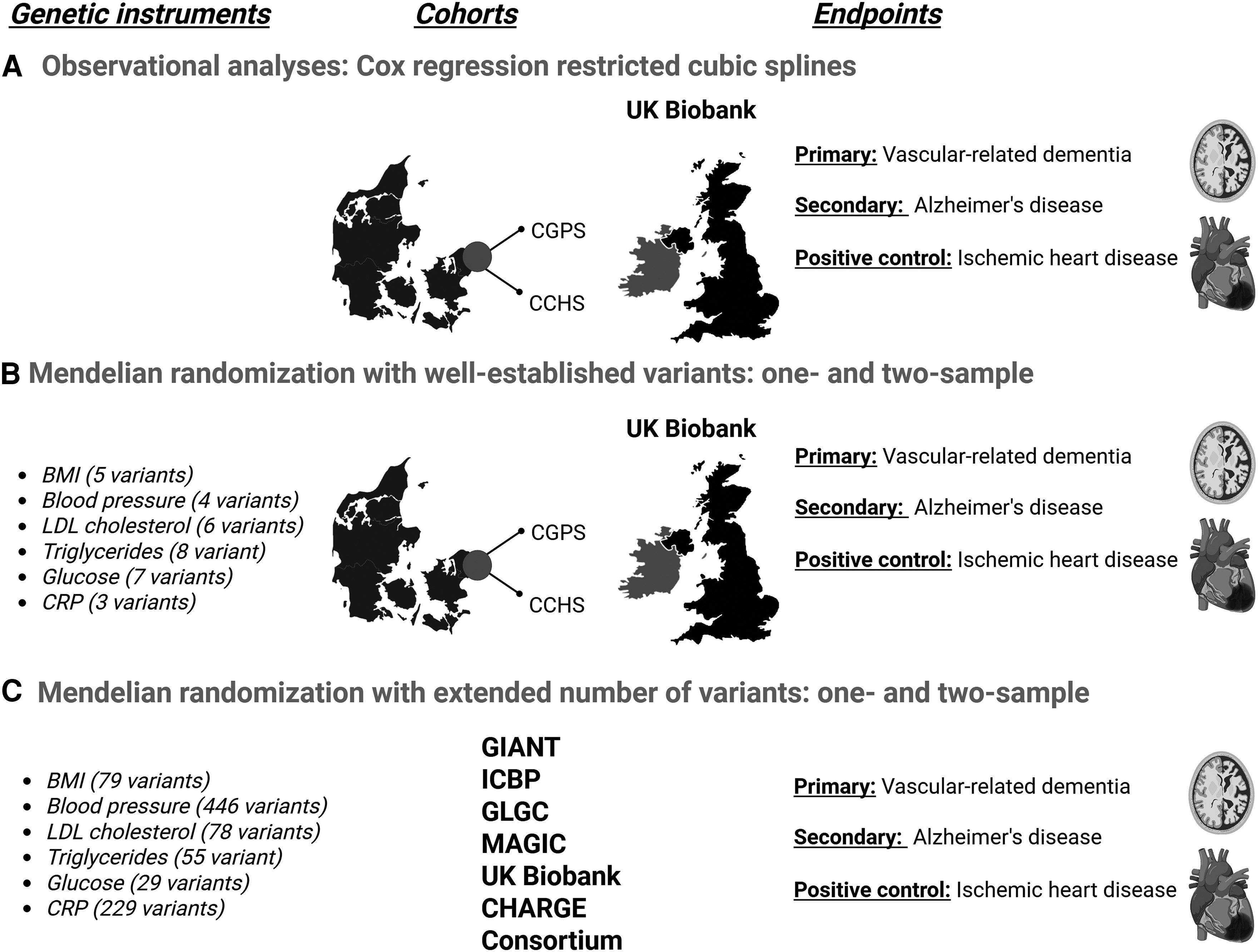
In this study, the BMI “instrument” was a genetic score built from 5 well-established variants.
To check that their MR approach was behaving as expected, they ran a positive control using ischemic heart disease, because higher BMI is already well-supported as causal for heart disease. If their MR approach failed to detect that known relationship, it would have been a major red flag (however, it performed as expected, validating their instrument).
Finally, they asked a mechanistic question: if BMI is causal, how much of its effect might operate through classic cardiometabolic pathways? They evaluated this potential mediation through blood pressure, LDL cholesterol, triglycerides, glucose, and C-reactive protein (CRP, commonly used as a measure of inflammation).
You just missed this in your inbox
Every week, Dr. Rhonda Patrick and the FoundMyFitness team distill the latest research into clear, actionable insights on health, longevity, and performance, delivered free to your inbox.
Higher genetically predicted BMI, higher dementia risk
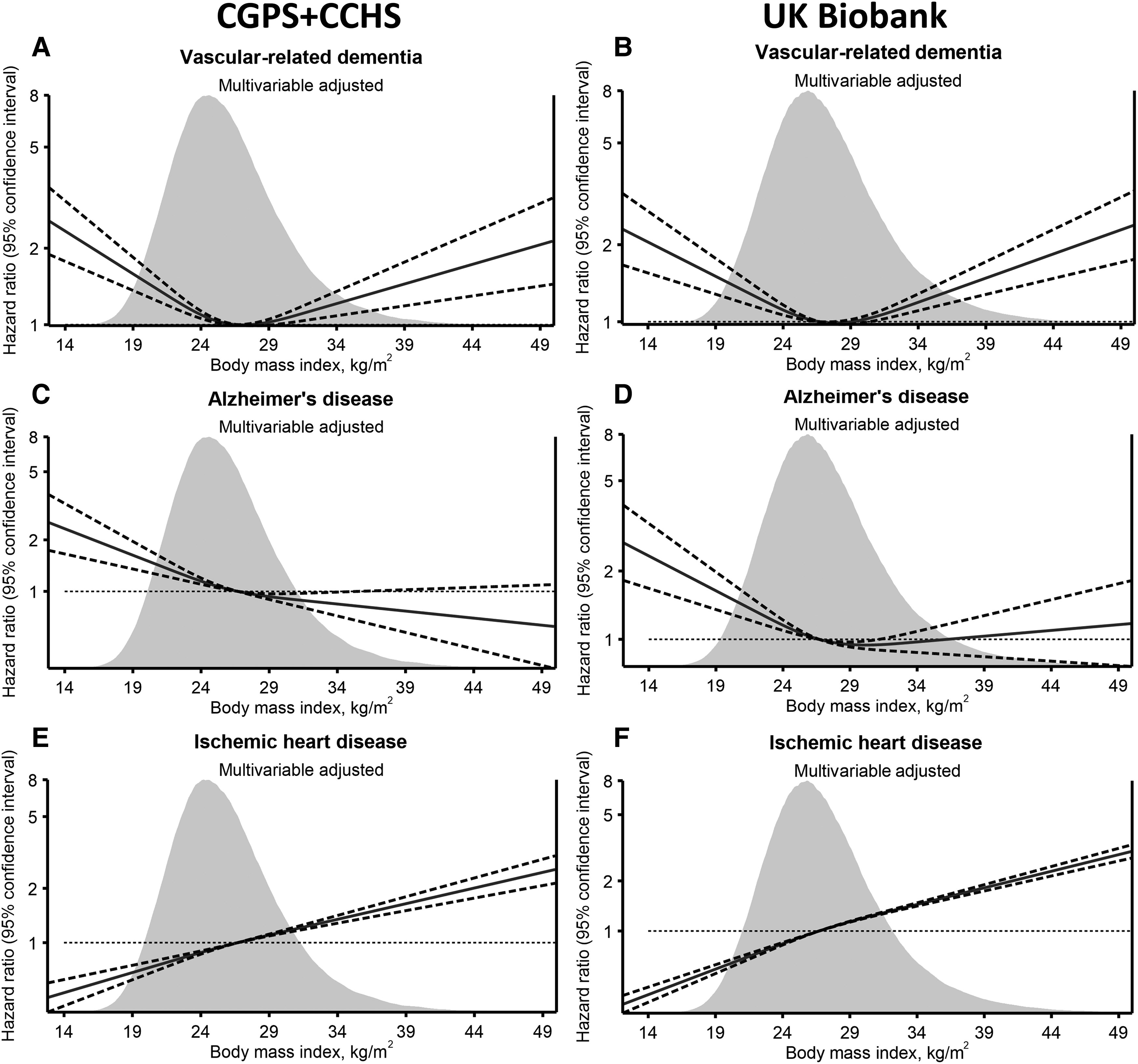
Observationally, BMI showed the classic U-shaped association with vascular-related dementia, with the lowest risk hovering around a BMI of ~27. That result isn't all too surprising given prior observational evidence.
|
|
The association between BMI and vascular-related dementia, Alzheimer's disease, and heart disease in the Danish cohorts (CGPS+CCHS) and the UK Biobank. |
But in MR, the relationship looked very different.
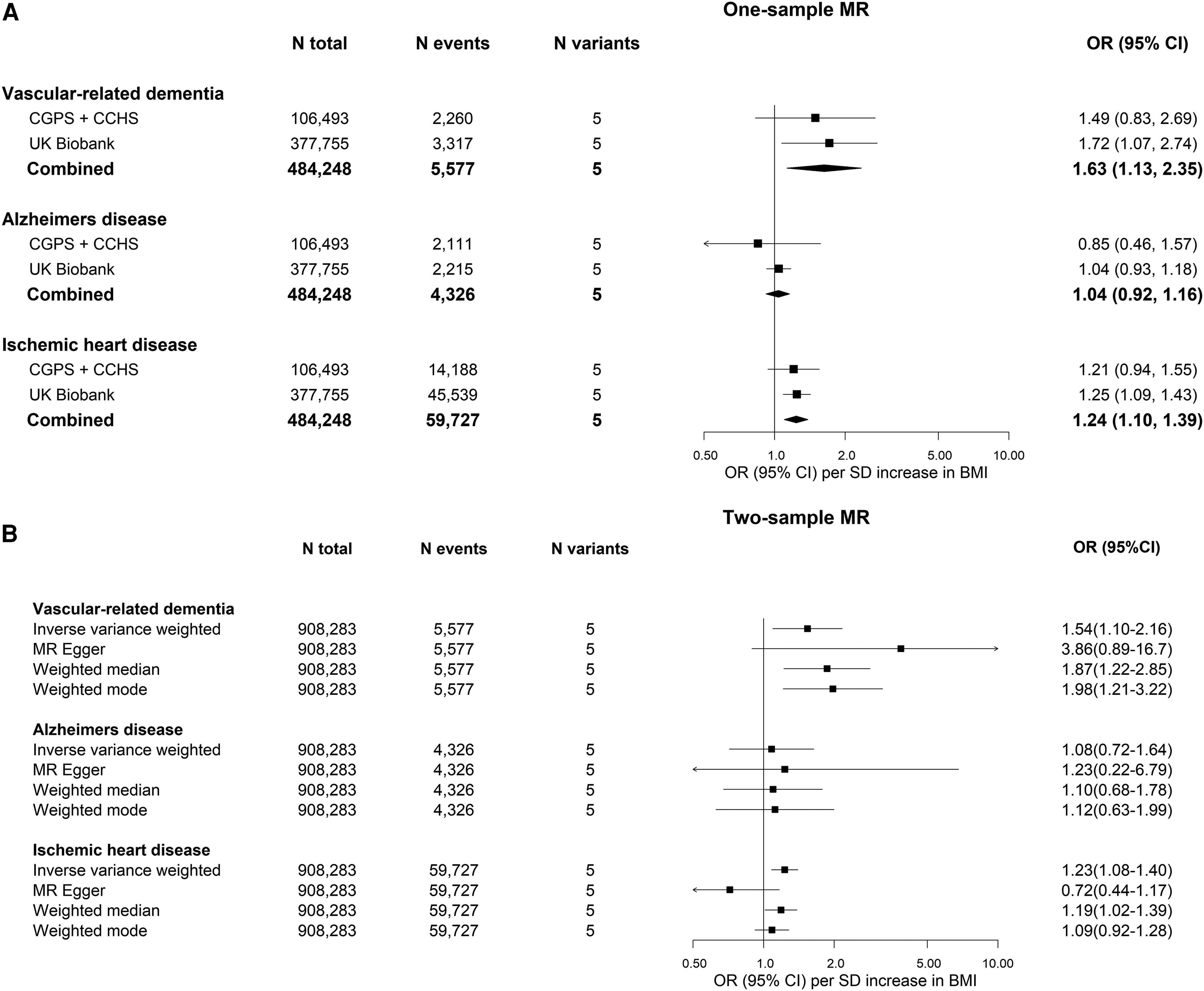
Genetically higher BMI was associated with a linear increase in vascular-related dementia risk—higher BMI, higher risk.
For every ~5 kg/m² increase in BMI (1 standard deviation), vascular-related dementia risk was 63% higher. A 5 kg/m² increase in BMI is equivalent to moving from normal weight to overweight or overweight to obese, which might be 30–40 extra pounds added for the person of average weight.
Notably, there was no association between genetically predicted BMI and Alzheimer’s disease risk.
|
|
The association between genetically-predicted BMI and vascular-related dementia, Alzheimer's disease, and heart disease risk. |
|
|
Blood pressure is the strongest intermediate risk factor
Before testing mediation, the researchers asked whether the cardiometabolic factors themselves were associated with vascular-related dementia risk.
Blood pressure was the clear standout:
An 18–24 mmHg increase in systolic blood pressure was associated with a 156% higher risk of vascular-related dementia. A 10–12 mmHg increase in diastolic blood pressure was associated with a 232% higher risk.
Glucose also showed a signal, with an 18–36 mg/dL increase in glucose associated with a 58% higher risk of vascular-related dementia. Meanwhile, LDL, triglycerides, and CRP weren’t clearly associated with vascular-related dementia risk in these analyses.
Systolic blood pressure was estimated to mediate 18% of the BMI-vascular-related dementia effect, while diastolic blood pressure mediated 25%.
The simplest interpretation here is that most of BMI’s association with vascular-related dementia is not “accounted for” by blood pressure alone, but blood pressure does explain a meaningful slice. It's a major pathway and seemingly more important than other well-established risk factors.
|

|
The association between genetically predicted systolic and diastolic blood pressure, LDL cholesterol, triglycerides, glucose, and CRP and the risk of vascular-related dementia. |
Why excess adiposity should raise dementia risk
Once you zoom out and look at mechanisms, it becomes much easier to understand why higher adiposity could elevate dementia risk, and much harder, if not impossible, to argue that low BMI should do the same.
There are multiple overlapping pathways by which obesity plausibly increases dementia risk over decades:
Obesity amplifies upstream vascular risk factors like blood pressure, insulin resistance, dyslipidemia, inflammation and oxidative stress, and sleep-disordered breathing—risk factors that slowly damage brain blood vessels over time. It also promotes endothelial dysfunction, impairing vasodilation and neurovascular coupling and increasing arterial stiffness. Over time, this reduces healthy brain blood flow and transmits pulsatile pressure into small vessels, classic substrates for white-matter injury and vascular cognitive impairment. And critically, endothelial dysfunction and arterial stiffness sit upstream of hypertension, which, based on today’s study, mediates a meaningful portion of the BMI-vascular-related dementia relationship.
(I discuss how high blood pressure causes dementia in this clip from my interview with Dr. Axel Montagne)
Fat tissue (especially visceral fat that sits on and around organs) produces pro-inflammatory cytokines that can sustain systemic inflammation, worsen endothelial dysfunction, and accelerate atherosclerosis. Systemic inflammation can also interact with microglia (the brain’s innate immune system), potentially accelerating neurodegenerative processes.
Insulin resistance and energy metabolism matter too. Obesity is strongly tied to insulin resistance and impaired energy metabolism. Neurons become less efficient at glucose utilization, which can reduce synaptic function. This may not fully explain vascular dementia specifically, but it’s a major pathway on the road to cognitive decline and other forms of dementia such as Alzheimer's disease.
Imaging studies add biological plausibility here. Higher BMI and body fat are associated with structural and functional brain patterns that fit what we already know about vascular cognitive impairment: smaller subcortical gray-matter volumes, altered white-matter microstructure, a higher burden of vascular injury markers like white-matter hyperintensities, and altered connectivity in networks involved in executive control and interoception/reward.
Put all of this together and the story becomes pretty intuitive: it's biologically plausible that excess adiposity increases dementia risk, especially via vascular pathways. It's much less plausible that low BMI is inherently harmful in the same way.
Which is why the “obesity paradox” often isn’t a paradox at all, it’s an observational artifact. And when you test the question with approaches designed to get closer to causality, like Mendelian randomization, that paradox tends to disappear.
|
 |
Final thoughts
This study reinforces something I’ve talked about for years: dementia prevention isn’t just about the brain—it’s about the blood vessels that feed it. Dementia is a vascular disease, and in this sense, excess adiposity isn’t just an issue of weight. It’s a decades-long (or more) vascular and metabolic stressor.
There are two ways we can interpret the study discussed today:
First, if you're overweight or obese, focus on losing weight safely and gradually. But don't hyperfocus on BMI—prioritize losing fat and maintaining lean mass, which can be accomplished with regular resistance exercise and adequate protein intake (I spoke with Dr. Luc van Loon about optimizing protein intake for muscle growth in episode #93 of the podcast).
Second, and perhaps more reassuringly, blood pressure is a lever you can pull (often quickly) and it matters for cognition. That doesn’t mean it’s the whole story, but it does mean that blood pressure is a highly actionable target for brain health. And importantly, it’s a target you can improve even if the scale doesn’t budge right away.
So what actually works to lower blood pressure, consistently, and with good evidence?
-
Aerobic exercise is one of the most reliable non-pharmacologic blood pressure interventions, and numerous studies link regular aerobic exercise with lower blood pressure and dementia risk.
-
Heat therapy (sauna or hot baths) can meaningfully reduce blood pressure by improving vascular function and inducing cardiovascular adaptations that overlap with moderate exercise. If you don’t have access to a sauna, hot baths can deliver many of the same blood pressure-lowering benefits when done regularly.
-
Sleep quality matters more than most people realize. Short sleep and sleep fragmentation raise sympathetic tone and worsen blood pressure control. If you snore loudly, wake unrefreshed, or suspect sleep apnea, getting evaluated is worth it.
-
Nutrition that improves insulin sensitivity also tends to improve blood pressure. Minimizing ultra-processed foods, emphasizing potassium-rich whole foods (like fruits, vegetables, legumes), and keeping an eye on excess sodium intake (especially in people who are sodium-sensitive) can all move blood pressure downward.
(Dr. Peter Attia explains his top strategies for reducing blood pressure in this clip from episode #85 of the FoundMyFitness podcast).
Your brain’s long-term fate is tightly coupled to the health of your vascular system.
If you’re thinking about dementia prevention, don’t just think in terms of memory. Think blood pressure, metabolic health, and vascular function. A blood pressure trend in the right direction is one of the clearest signals you can get that you’re reducing one of the most important modifiable risks for cognitive decline.
|
Warm regards
— Rhonda and the FoundMyFitness team
|
|
|
|
|
|