 |
The consistency of your sleep schedule could be nearly as important as the total hours you sleep each night.
According to new research, people with highly irregular sleep patterns are at a 26% greater risk for heart attack, heart failure, and stroke compared to more consistent sleepers. Among moderately irregular sleepers, the risk of cardiovascular events increases 8%.
More concerning is that an inconsistent sleep pattern elevates cardiovascular risk even in people with a sufficient sleep duration. Let me repeat that: Sleeping enough does not offset the negative effects of an irregular sleep pattern.
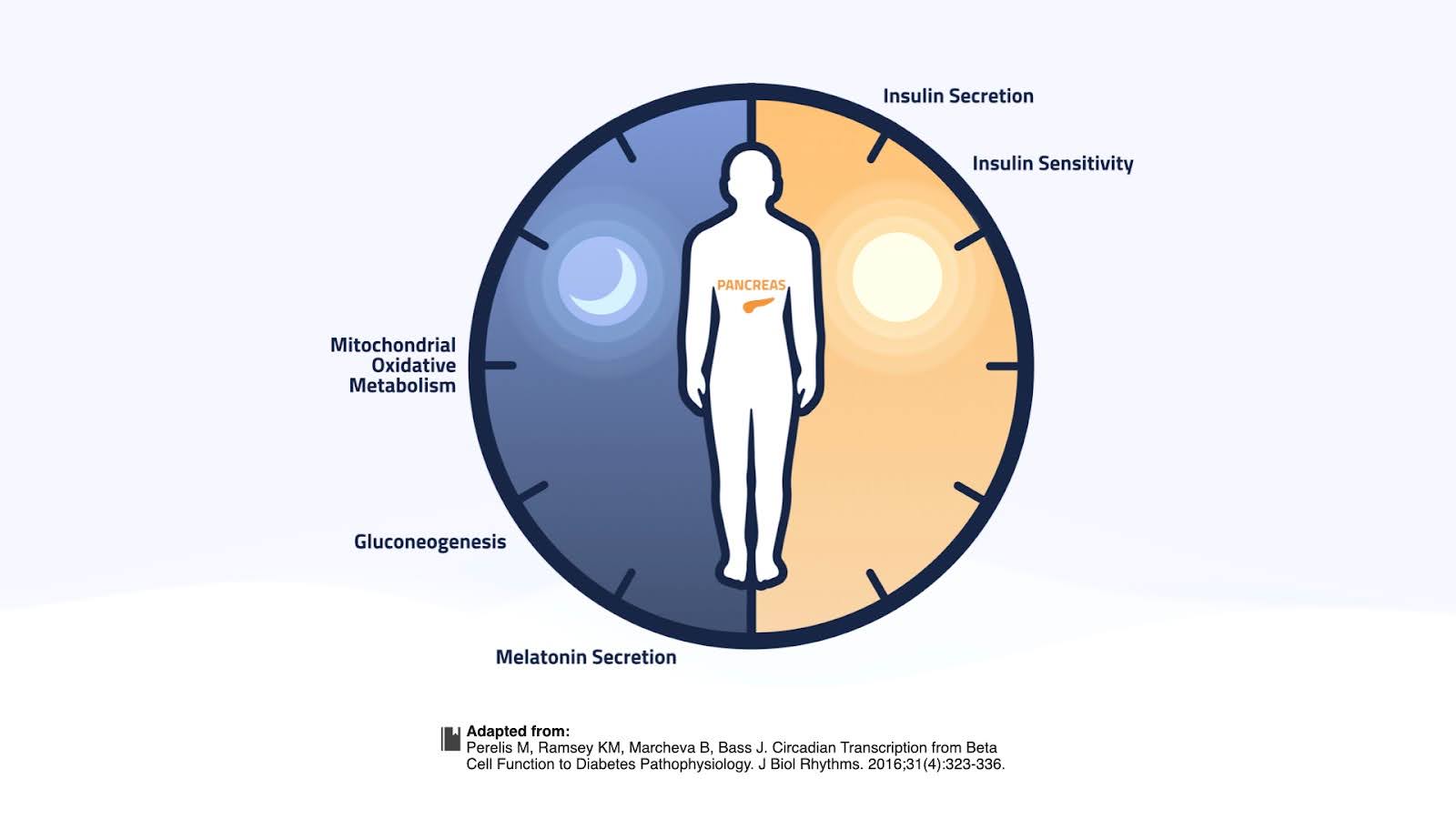
This is likely because erratic sleep patterns disrupt circadian rhythms, the internal clocks that govern critical processes like metabolism, hormone release, and even cognitive performance.
This applies to meals too. Eating out of sync with our body's circadian rhythms in metabolism and melatonin release causes glucose dysregulation—a risk factor for diabetes. This is why time-restricted eating (TRE) is so beneficial.
A new study suggests that shifting sleep and meal times by 5 hours (a form of social jet lag) can lead to changes in metabolic physiology—after just one day, digestion was slower and blood glucose control was worse after meals. This was accompanied by a decline in alertness levels and greater sleepiness, changes that persisted for up to 5 days.
These findings are concerning because they suggest that social jet lag that we experience on the weekend or real jet lag during time-zone travel may have profound effects on our metabolic function.
In today's email, we'll explore this study in an attempt to underscore why timing is of the utmost importance for health and what it means for you.
|
|
You just missed this in your inbox
Every week, Dr. Rhonda Patrick and the FoundMyFitness team distill the latest research into clear, actionable insights on health, longevity, and performance, delivered free to your inbox.
The consequences of delaying bedtime and meals
The participants in the study underwent an experimental procedure known as forced desynchrony—the researchers manipulated their sleep-wake, light-dark, and feeding-fasting schedules in a way that misaligned their internal circadian rhythms (i.e., in metabolic function and hormone release) with external cues (light, sleep, and food).
This was accomplished by delaying bed times and meal times by 5 hours for a total of 5 days.
Whereas participants normally woke up around 7 am and went to bed at 11 pm, the phase-shift protocol called for a 4 am bedtime and a wake time of noon, though they were still allowed their normal 8 hours of sleep per night. Sleep timing changed while sleep duration didn't.
Meal times were also disrupted—breakfast, lunch, and dinner occurred at 1 pm, 6 pm, and 11 pm compared to the normal times of 8 am, 1 pm, and 6 pm. However, what and how much the participants ate was kept consistent.
Even though sleep duration and diet were maintained, the 5-hour phase shift resulted in some acute—but not lasting—changes in metabolism that manifested in less than one day!
Phase shifting hampers glucose control and digestion
One of the most notable changes was a slowing of digestion after breakfast.
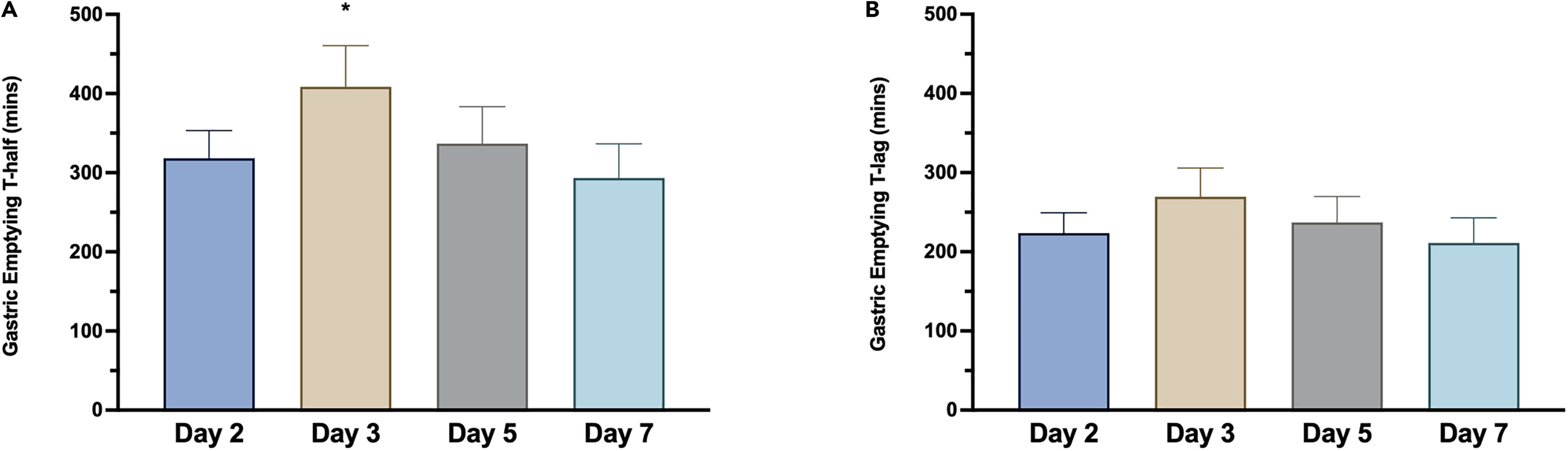
After just one day of eating later than usual, participants experienced a 90-minute delay in gastric emptying—proof that their bodies weren’t prepared to break down food efficiently. The hormonal and enzymatic systems had yet to adjust to the change.
Glucose and triglyceride levels rose significantly across breakfast, lunch, and dinner even though fasting blood glucose levels dropped on days 1–3. Poorer glycemic control appeared to be the most pronounced at breakfast. However, daily glycemic variability (measured using continuous glucose monitoring) wasn't affected—the biggest metabolic impact comes right after eating.
While the metabolic shifts happened quickly, they didn't appear to last. Once the participants started to adapt to the phase delay—when levels of melatonin, sleepiness, and alertness realigned with their new schedules—so did their metabolic responses to meals. This occurred between days two and three of the study.
|
|
Gastric emptying rate is slower on the first day of the phase shift (day 3).
Alertness and wakefulness levels decline while metabolism is unchanged
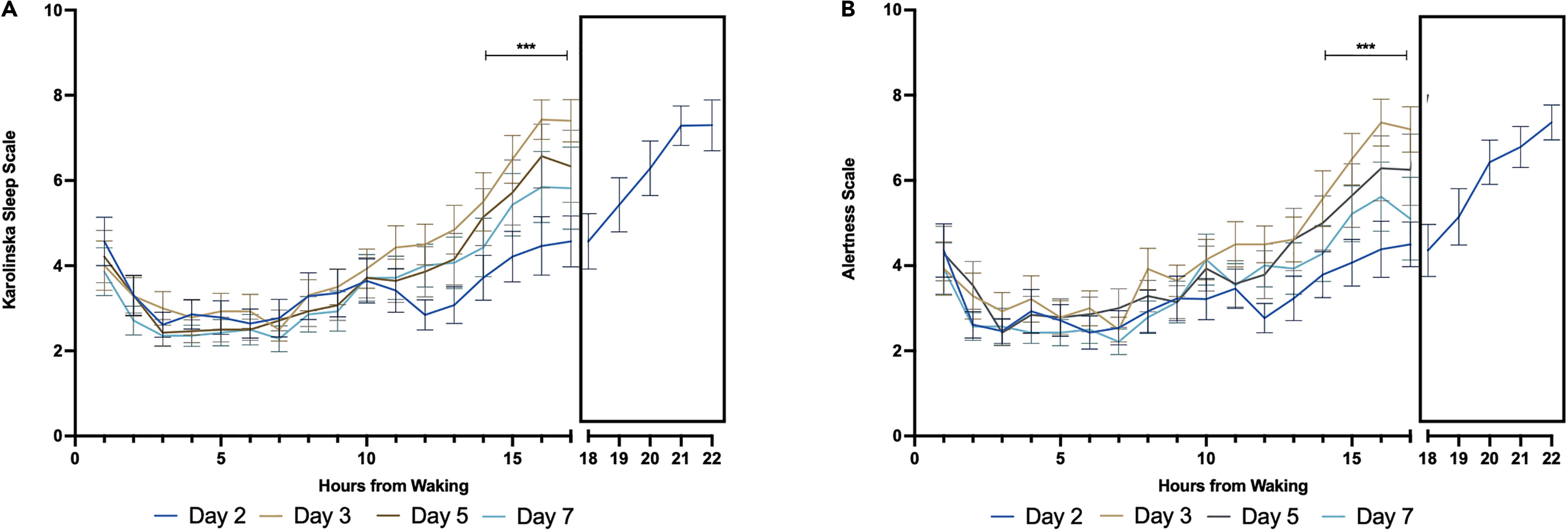
Participants also reported feeling sleepier and less alert in the afternoon and evening following the first day of the phase shift. They had sleep-deprivation-levels of alertness and tiredness even though they weren't sleep deprived. Unlike the metabolic responses to the phase delay—which worsened after a single day but returned to baseline after 3 days on the new schedule—sleepiness and alertness levels were continually impaired for up until the fifth day of the shifted schedule.
Therefore, while metabolism might adjust more quickly to changes in sleep and meal timing, the brain may take longer to adapt.
The phase shift did leave some aspects of metabolism unaffected, however. Resting metabolic rate, total daily energy expenditure, and even the post-meal increase in metabolic rate (known as the thermic effect of food or TEF) didn't change after the shift in behaviors occurred. Neither did hunger levels, fullness levels, or appetite throughout the day.
|
|
Levels of sleepiness (left) and alertness (right) are reduced on days 1-5 of phase-shifting.
Final thoughts
Does this mean that you can never have a late night out with friends or let yourself sleep in on the weekends? Of course not. We have to live life with room for fun and flexibility.
However, these results probably explain part of why we don't feel as good when we go to bed at an odd time, sleep in until noon, or eat a late-night meal—our body just isn't primed (from a chronobiological perspective) to handle this quick shift. Maybe you've experienced a drop in wakefulness and alertness from social jet lag. Or maybe you've felt like your digestion was a bit off after traveling across a few time zones. These feelings make sense when you consider that the body needs time to adjust metabolism, hormone release, and cognitive functions to the new time zone before you feel "normal" again.
We all may unknowingly be inserting some social jet lag into our own lives. It's probably not uncommon for most of us to shift our sleep and meal patterns by 2–3 hours on occasion—on the weekend, perhaps.
It's okay when this happens, but the important thing is not to make it a habit. Interestingly, this study showed that we might eventually adapt (somewhat) to a new schedule, but the reality is that when most of us experience social jet lag, it's only for a day or two—not 5 days like in this study. We eventually revert back to our usual routines. This constant flip-flopping is not good for our metabolic health.
The actionable take away here is this: Go to sleep, wake up, and eat your meals at virtually the same time every day.
The body craves consistency. And when it gets what it craves, it rewards us with good health.
To improve sleep consistency and optimize both performance and longevity, here are 10 practical strategies grounded in the latest research and circadian biology:
- Stick to a consistent schedule by going to bed and waking up at the same time daily, even on weekends.
- Get morning light exposure by spending 10–30 minutes in natural light within 1–2 hours of waking to anchor your circadian rhythm.
- Limit evening light exposure by reducing artificial light 1–2 hours before bed and using dim, warm lighting or blue-light-blocking glasses.
- Time meals wisely by avoiding heavy meals within 2–3 hours of bedtime to prevent circadian disruption.
- Exercise earlier in the day and avoid intense workouts close to bedtime.
- Optimize your sleep environment by keeping your bedroom cool, dark, and quiet, and consider using blackout curtains or white noise machines.
- Limit stimulants like caffeine after mid-afternoon and minimize alcohol to protect sleep quality.
- Create a wind-down routine with relaxing activities like reading, meditation, or light stretching before bed.
- Manage stress by practicing mindfulness, deep breathing, or journaling to reduce pre-sleep anxiety.
- Avoid sleep disruptors by limiting naps to 20–30 minutes and reducing fluid intake 1–2 hours before bedtime.
For more on sleep, including supplements that might benefit sleep quantity and quality, check out these member Q&A episodes and their accompanying shownotes which we've enhanced for your learning pleasure!
|
Q&A #53 with Dr. Rhonda Patrick (11/4/2023)
-
28:27 - Rhonda's "sleep stack"
-
30:35 - Does magnesium threonate improve sleep?
-
32:56 - Does apigenin enhance sleep? (and good sources without supplementing)
-
34:52 - Which supplement has the best evidence for improving sleep: magnesium, apigenin, or l-theanine?
-
35:43 - Struggle with sleep? This is the number one thing you should try
-
36:13 - Can magnesium threonate be taken long-term?
-
37:13 - Do myo-inositol, GABA, and glycine help sleep?
-
38:07 - The most bio-available magnesium supplements
|
| |
|
Q&A #29 with Dr. Rhonda Patrick (11/6/2021)
-
18:52 - Do magnesium threonate, apigenin and l-theanine improve sleep?
-
19:18 - The limited data on magnesium threonate for sleep
-
21:26 - Why chamomile tea could improve sleep quality
-
23:11 - Theanine's sleep efficiency & quality benefits
-
24:32 - Is magnesium malate superior to other forms of magnesium?
|
| |
|
With appreciation,
Rhonda and the FMF Team
|
| |
|
|
|
|